 Please don’t have to bring out your dead.
Please don’t have to bring out your dead.
Written By:
- Date published:
12:27 pm, March 29th, 2020 - 45 comments
Categories: covid-19, Economy, health, Social issues, tourism, uncategorized -
Tags: epidemic, future, pandemic
Anyone who has read even briefly into written human history is going to be aware that it is as much defined by our epidemics and pandemics as by any of our technical and societal achievements. This post is essentially a quick range over the history of pandemics and epidemics with links and some focus on COVID-19.
The effects of pandemics is apparent in the written accounts of the Plague of Justinian which winnowed the Eurasia and Africa for from the 6th century and variations repeating to the early 20th century Or the undocumented plagues that repeatedly decimated or destroyed civilisations in the Americas prior to European invasions. Or the plague disasters that followed the colonial empires spreading regional diseases on a grand scale keep reverberating in indigenous populations to the present day.
Most of the diseases that have been common through human history have had their impacts constrained with the awareness of the sources of epidemic diseases, the introduction of better sanitation, the long slow history of developing vaccines, and effective preventative medical treatments.
But through the 20th century, at least in developed world, the ever-present dread and awareness of epidemics that was still residual during my childhood in the 1960s has dissipated. My grandparents lived in aftermath of the 1918 influenza pandemic. My parents grew up as the polio epidemic was attacking their classmates. During my childhood there were continuous mini-epidemics of various infectious diseases from mumps to measles.
Our generations saw the effect of the introductions of vaccines and the loss of knowledge about epidemics in our society diminished.
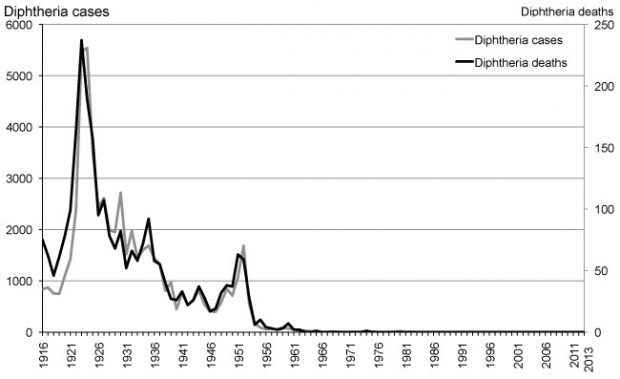
As an example in my life, diphtheria was a disease that well known to my grandparents and parents. But it was disease that I had no idea about. The vaccine was introduced into NZ in 1941 for children under 7 well after the 1921 epidemic. This graph from a 2016 post by Helen Petousis-Harris at Te Pūnaha Matatini “If only there had been a vaccine” displays clearly why I wasn’t aware of it – I was born in 1959.
When I’ve talked to my younger relatives and colleagues, their ignorance of the dangers of diseases that were worried the hell out of my parents when I was growing up is just scary as hell. They simply don’t feel the fragility of the clean water systems that we depend on to stave of outbreaks of diseases like cholera, or why using antibiotics blithely for viral diseases or milk production is a stupid idea, or why using vaccines isn’t an individual choice like what brand of cellphone you like.
This ignorance has been particularly apparent to anyone who has spent time online looking aghast at the deliberate spreading of misinformation by anti-vaxxers over the last decade. Instead of the ever-present dangers of re-emerging diseases, recent generations seem to be more invested in the fantasies of the zombie apocalypse rather than the more mundane concerns about rubella or measles.
Virtually all of the epidemics that have a potential of flaring into pandemics now appear to be emerging infectious diseases especially those noted as being ‘novel’ or previously unknown to our medical histories.
Emerging infectious diseases are infections that have recently appeared within a population or those whose incidence or geographic range is rapidly increasing or threatens to increase in the near future. Emerging infections can be caused by:
- Previously undetected or unknown infectious agents
- Known agents that have spread to new geographic locations or new populations
- Previously known agents whose role in specific diseases has previously gone unrecognized.
- Re-emergence of agents whose incidence of disease had significantly declined in the past, but whose incidence of disease has reappeared. This class of diseases is known as re-emerging infectious diseases.
The World Health Organization warned in its 2007 report that infectious diseases are emerging at a rate that has not been seen before. Since the 1970s, about 40 infectious diseases have been discovered, including SARS, MERS, Ebola, chikungunya, avian flu, swine flu and, most recently, Zika.
With people traveling much more frequently and far greater distances than in the past, living in more densely populated areas, and coming into closer contact with wild animals, the potential for emerging infectious diseases to spread rapidly and cause global epidemics is a major concern.
To that list, we can now add severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) – the virus strain that causes COVID-19. This is probably a well established viral disease in bat populations that has recently made the jump to humans via an immediate species.
Inter-species crossover has been a common theme in novel infectious diseases. HIV probably crossed over from chimpanzees in the early 20th century. MERS is probably a crossover from camels. Ebola probably also from bats via infected apes. Avian flus mostly from from birds and swine flu mostly from pigs as their names indicate.
The issue with novel diseases is that when they do managed to have an inter-species crossover that allows for a successful intra-species infection in humans, they are sometimes extremely infectious. Frequently they’re so infectious that they are self-limiting.
Ebola is like this. When it gets into a susceptible population with poor medical support with social hygiene and customs that facilitate immediate transmission, the outbreaks burn themselves out fast. That is because the association between caring for patients or grieving for the dead becomes obvious within a short period to survivors.
This is a self-limiting strategy for the disease. To date Ebola has had limited success infecting anyone outside of central Africa despite a number of infected travellers, particularly in 2014.
The 2003 SARS outbreak was contained primarily because the number of people with mild symptoms were low. It also did not have a . This made isolation of the infected, the containment and testing of people that were associated with, and the eventual eradication of the disease feasible. But there was also a healthy dose of just luck as a World Health Organisation after-action-review made clear:-
The rapid containment of SARS is a success in public health, but also a warning. It is proof of the power of international collaboration supported at the highest political level. It is also proof of the effectiveness of GOARN in detecting and responding to emerging infections of international public health importance. At the same time, containment of SARS was aided by good fortune. The most severely affected areas in the SARS outbreak had well-developed health care systems. Had SARS established a foothold in countries where health systems are less well developed cases might still be occurring, with global containment much more difficult, if not impossible.
Although control measures were effective, they were extremely disruptive and consumed enormous resources — resources that might not have been sustainable over time. If SARS reoccurs during an influenza season, health systems worldwide will be put under extreme pressure as they seek to isolate all those who fit the clinical case definition until diagnosis can be ascertained. Continued vigilance is vital.
This chapter has illustrated how quickly a new disease can threaten global health. Thankfully, not all diseases move at such speed; but some are more stealthy and more lethal.
The SARS epidemic was contained within 12 months. Which in retrospect was somewhat unfortunate. Most of the advanced efforts to get an effective vaccine or treatment against SARS were shelved as the epidemic was being contained or in the decade following in a classic case of failing to be actively proactive after a scare.
There are a number of vaccines that were developed. Many of which had issues with the effect of the vaccine causing over-energetic responses in test subject’s auto-immune systems and increased symptoms. Unfortunately excessive auto-immune responses are also the main cause of fatalities with both SARS and COVID-19.
The COVID-19 is in many ways similar with the 2003 SARS outbreak as this Lancet article “Can we contain the COVID-19 outbreak with the same measures as for SARS?” but has some differences that make it far more stealthy.
Clear differences are emerging, such as in transmissibility and severity pyramids; COVID-19 has a higher transmissibility than SARS, and many more patients with COVID-19 rather than SARS have mild symptoms that contribute to spread because these patients are often missed and not isolated.
Mild symptoms with COVID-19 are really really problematic for containment because of the viral shedding as this quotation from the Lancet article makes clear (my italics).
Isolation was effective for SARS because peak viral shedding occurred after patients were already quite ill with respiratory symptoms and could be easily identified. Although asymptomatic or mildly symptomatic patients have been reported for SARS,35 no known transmission occurred from these patients. By contrast, preliminary evidence from exported COVID-19 cases suggest that transmission during the early phase of illness also seems to contribute to overall transmission;36, 37 therefore, isolation of more severely ill patients at the time of presentation to health-care facilities will be too late. The effectiveness of isolation and contact tracing methods depends on the proportion of transmission that occurs before symptom onset. Pre-symptomatic transmission will also make temperature screening less effective.38
In other words, with COVID-19 you can be infected with few or even no symptoms and still infect others as a carrier. With SARS it could be contained because people who had it were symptomatic and infectious or non-symptomatic and apparently not infectious. What is also known is that people who have gotten over the disease can also shed viruses for some time afterwards. The European CDC says in their discharge criteria
SARS-CoV-2 virus can initially be detected 1–2 days prior to symptom onset in upper respiratory tract samples; the virus can persist for 7–12 days in moderate cases and up to 2 weeks in severe cases (WHO mission to China Report) [1]. In faeces, viral RNA has been detected in up to 30% of patients from day 5 after onset and up to 4 to 5 weeks in moderate cases. The significance of faecal viral shedding for transmission still has to be clarified [1].
In the absence of a vaccine or preventative treatment, the mild symptomatic infection and potentially long shedding periods mean in most places containment is likely to fail as strategy.
While potential for fast report antibody tests will capable of detecting if someone has contacted the disease. However as the New Scientist and others pointed out
If we know someone has had the virus, they can potentially leave their home without risk of being re-infected, which would help countries get moving again. However, the accuracy of the tests has yet to be established. “The one thing that’s worse than no test is an inaccurate test,” Chris Whitty, the UK’s chief medical adviser, said on 25 March. Someone wrongly told they have already had covid-19 could go out and get infected.
and
The antibody response to the coronavirus may be delayed compared with other infections. The tests can be used only 14 days or more after people develop symptoms, says Adams.
This also means antibody testing will be of limited use for tracing the contacts of infected people – which many think is crucial for controlling the outbreak – because health authorities will be weeks behind.
Plus a positive antibody test doesn’t indicate where people are in the virus shedding cycle. Currently only a swab test taken by trained personnel and sent to lab for analysis will do that.
Which makes Boris Johnson’s enthusiasm for the antibody test (even assuming it works as advertised) as being ‘game-changer’ ridiculous. It serves more as an indication of his habit of being a dangerously ignorant idiot. The New Scientist article ends with a better informed and thought through analysis..
On the plus side, many groups are working on faster genetic tests and on antigen tests that can detect the virus in, say, saliva. Testing widely for both active infections and past infections should be a highly effective combination.
Of course to make that work for getting people back into the workforce, we’d probably need to bulk-order bracelets to allow confirmation for people who can be out and about because they neither get nor infect with the virus. I’d imagine that in NZ that being required to carry infection status identity will, in itself, cause some debate.
However in New Zealand we have what Jacinda Ardern describes as a “reasonable” chance of doing a containment strategy. Closed borders apart from those kiwis and their spouses and dependents still able to make it back, a slowly increasingly strict isolation policy for arrivals, and a lock-down for 4 weeks make it possible.
My background as a part-time army medic and as a lifelong student of the history of epidemics makes me want to get somewhat draconian.
For travellers arriving, our continuing primary disease vector, we should use the isolation model that Taiwan has been using. Ensure that people in isolation have food delivered and don’t have to leave. If they are in a hotel or home then require active tracking the GPS of phones, and regularly and randomly auto-poll that phone to make sure that the owner is next to the phone. One article I read on Medium which I can’t find now described the wakeup call that one taiwanese arrival got when their cellphone battery ran out of power and they had police banging on their door shortly afterwards.
If people don’t follow the common sense rules for isolation to prevent the spread of infection, then I’m sure that we can find an island and a tent to drop them on for a month until the court has time to deal with them. At the very least it will prevent them to be being a stupid danger to others.
I’d suggest that the same happens to the owner or manager of businesses who self-deem themselves to be ‘essential’. Not only are they putting customers in danger, but presumably they’re also pressuring employees to do it as well.
The biggest problems for NZ with our current strategy is to prevent issues with community transfer during and after the release of the lockdown. This would result in lockdowns extending or resuming in areas – often far wider than local areas.
So far I’m not optimistic that a single national lockdown will be completely effective because people seem to be taking some very liberal interpretations of what a household ‘bubble’ means. There are anecdotal reports of household bubbles joining up so that their kids can play together. Or kids playing games in parks. Its going to be interesting see how this plays out in the coming weeks. Each of these effectively widen out any lockdown to quarantine outbreaks.
Hopefully someone has started to do location tracking on cellphones to find out what are actual ‘local’ areas as evidenced by actual aggregate movements.
If our containment strategy does work and community spread is eliminated. Then the big question is – how we reconnect to rest of the world?
We’d wind up with a small number of immune people and most people being susceptible. At the very least, we’d need to have border antibody and live virus tests before people boarded and a rapid retest on arrival. Validation of the error rates on combinations of tests will determine the risk levels. Otherwise tourists, business travel, and returning kiwis will require 14 days quarantine.
Our tourist industry will be hanging out for a vaccine in NZ. Realistically before we can start up Hobbiton we’d require a largely immune population.
As importantly, before we restart our tourism industry or to allow kiwis to fly offshore again, we’re going to need to have a very close look at how we deal with the next ‘novel’ disease. I, for one, have absolutely no real interest in dying for tourism.
Basically we are trying to do with our containment strategies is to avoid the modern analogue in a covid-19 Italy and elsewhere of “bring out your dead”. This was the defining civic characteristic of past pandemics.
In Italy, as the fatalities of covid-19 overwhelm the funeral systems we get the military being called in to transport the dead.
At least it is a bit more civilised and dignified than the black humour of Monty Python’s depiction of the same task in a medieval plague.
Anything is better than that.
45 comments on “Please don’t have to bring out your dead. ”
- Comments are now closed
- Comments are now closed

Thank you LPent.
I'm a bit older than you, Lynn. I remember queuing up at primary school for a polio vaccine (oral) and BCG test for TB. the TB test involved being kind of stamped with multiple skin pricks in one shot, on the wrist.
I recall being scared when I heard an adult down our street was partially paralysed as a result of polio. Eventually I confided my fear in my mother at bedtime. She reassured me I wouldn't get it, cos she and Dad hadn't got it, etc.
The first couple of times I travelled overseas, I had cholera injections, and small pox scratch-type vaccines on my shoulder – still have the scar. Whilst travelling the cholera shots had to be renewed about every 6 months, and recorded on my vaccination card.
Disease outbreaks were pretty common in the UK and Ireland in the 19th century (open sewers were a cause) – worst was during the potato famine in Ireland when typhus was rife there.
Typhoid also was one of the factors that ended the dominance of classical Athens – due to unhealthy sanitation – throwing slops and sewage out windows, etc.
These are the reasons why we have our current sewage and rubbish collection systems.
I imagine the 21st century viruses will result in preventive systems being developed, domestically, and in relation to overseas travel. Our border control systems will change long term. And probably we will end for good, hand shaking, travelling about town when sick, packing people like sardines into mass transport services, etc.
As a result of my experiences in my younger days, I take preventive measures seriously.
We didn't stop any of that after Sars, Mers and other sars virus that we don't hear of that were not so viable, and like all those with a bit of luck this Sars virus will die out too. It is mainly because it needs a host to remain viable and can only remain viable for hours or days at the most outside the human body. The problem will be if it can remain viable long term in those who are immune to it but so far that does not seem to be happening. It spread in Wuhan because it was given time to be hosted by thousands and spread worldwide within that time.
That is why all the talk is about breaking the chain. We are lucky here that this brilliantly led Government is taking the best advice possible and treating it with the respect it deserves unlike most of the incompetent right-wing dickheads in the rest of the world.
I am thinking of preventive measures to prevent further outbreaks of new viruses. I understand places like Sth Korea already had systems and resources in place after the initial SARS outbreak, focused on responding quickly to any new viruses that may arise. So they were able to respond quickly to Covid-19.
Exactly Carolyn, I don't think we thought this one would get this far but I'm pretty sure a certain level of preparedness is/was in place. The difference for this mongrels spread is that it is "silent "for up to five days or longer while being diffused through the community, which the experts don't think had been happened before in Sars like pathogens.
I'd like to think that the answer to it may lie in why others can seem to fight it off sometimes without even knowing it. I bet researchers are looking there already.
As I pointed out in that long post, that is part of the problem. From the viruses 'perspective' having the host running their immune system ‘hot’ or even dying on it while it is breeding is a bad bet.
From my reading on covid-19, the thing that causes most of the nasty symptoms and death appears to be your own immune systems trying to deal too strongly with an intruder too late. That is what gives you the really bad cough and sneeze reflexes to clear viruses out of the lungs. It is what causes the lung inflammation which appears to be the usual cause of death.
The elderly have on average more sluggish immune systems. They react much slower to bugs and viruses. Moreover their immune systems frequently overreact especially with lung inflammation.
Younger people without compromised immune systems are faster reacting to catch the invading virus and triggering the second tier of immune responses (ie past the initial layer of fever, coughing, and sneezing) earlier and preventing a build up of virus load.
Problem is that while some people may only be mildly symptomatic, they’re still trailing a trail of generated viruses for many days after their symptoms die down. Unfortunately that really just means that they’re more productive at breeding the virus because they will usually wind up infecting more unsuspecting people they come into contact with.
Imagine if Joyce and his cronies were still in charge? Or Bridges for that matter. Even when it's clear Australia, US and the UK have missed the boat we're still being told this sort of shit. Hopefully, when this is all over, the lunacy of the right will become apparent to the general population:
https://www.stuff.co.nz/national/politics/opinion/120649991/how-will-we-exit-the-lockdown
I don’t think you can dismiss what Steven Joyce has written as shit. The economic cost of this shutdown will be massive, and as usual those on lower incomes will be hardest hit. It will be almost as important as the timing of the start of the shutdown as when we decide to finish it, or scale it back.
These things do need to be considered fairly soon to have some sort of plan trying to get back to normal.
Sure, the timing of the end of the shutdown will be important, but Joyce is suggesting starting to open things up at the end of the four weeks unless it's clear things aren't improving – a slightly watered down version of what Trump's been saying up until his recent change of tone.
The innumerate Stephen Joyce?
No fan of Joyce but the article seems reasonably reasonable.
Pretty legal, you think?
I'm the same age as Lynn, by the way, but had much the same experiences as you.
My mother had polio during the epidemic. She was one of the fortunate ones. They both tell me how scary it was hearing about classmates dying.
Actually, on further thought I think I had the test and oral vaccination at secondary school – maybe 3rd form. So those of you a bit younger may have had them at primary school.
I think our parents went through some tough times in the 1920s-50s.
Staying a home, physical distancing, loss of income still probably very tolerable for many of us. As always, it is those on low incomes and with underlying health issues that we need to support. Let's hope the majority of the country step up to do that.
What seems to be lacking at the moment is any evidence of human immunity developing to covid-19. Without immunity we will continue to be hit again and again, and isolation efforts will only delay the inevitable.
Death is inevitable for all – in a Covid-19 context, delay has much to recommend it.
The fact that people are recovering means their immune systems are working and developing immunity.
What is unclear is how long that immunity lasts, and/or how quickly the virus evolves to the point of being able to re-infect someone that had previously developed immunity.
While it is indeed possible that we'll have to deal with repeating waves of equal (or worse) severity, what is far more likely is that some degree of immunity will develop and future waves will be less severe. It's also reasonably likely that with enough time vaccines and/or pharmaceutical therapies will be developed. Then the usual evolution trajectory for infectious diseases is to become less harmful – it's really not beneficial for an organism to kill its host.
This virus, like all coronaviruses, mutates and over time, it might become less harmful. In practice, this could mean that it will travel around the globe causing seasonal spikes in disease and deaths, just like ordinary flu.
Depends on the rate that covid-19 'mutates' (actually mostly how often it incorporates other species rna).
Influenza is a promiscuous as hell. So far the SARS-COV-x viruses don't appear to be.
Long may that continue…
https://www.stuff.co.nz/national/health/coronavirus/120656955/eight-strains-of-the-coronavirus-are-circling-the-globe-theyre-giving-scientists-clues
A nice read, even for a non-science audience.
yeah it was a good article and a good site NextStrain.org
Try hitting the play button on… https://nextstrain.org/ncov
A charming tale.
https://nymag.com/intelligencer/2020/03/the-story-of-a-coronavirus-infection.html
https://en.wikipedia.org/wiki/Jeff_Wise
From an historical perepective have a read of Pepys Diary during the plague years, 1665/1666
http://www.pepys.info/1665/plague.html
"I, for one, have absolutely no real interest in dying for tourism."
I think you're not alone in that sentiment. Even family members who work in the tourist industry are questioning its future viability/validity.
An interesting point raised in the book Justinian's Flea is the relationship of the rise of the plague, and a extended period of warmer temperatures. We are set for a very extended period of warmer temperatures, I don't like our prospects.
I also don't like our prospects of keeping isolation down here at the bottom of the south seas. We lack some basic industries to be isolated. My hope is out of this, we start building some self–sustaining industry here for ourselves.
I agree with DV Iprent, and thank you. It has clarified a lot of issues for a thick clod like myself.
Because of the lower numbers now entering the country why are they not all being tested. Are we ( the Government) that dim.
I can't speak for the government's reasoning, but for my reckons:
Detecting community transmission and stopping it is a big factor in determining when we can drop alert levels. We have limited testing resources, so it seems to make most sense to use it for detecting cases that transmitted within New Zealand, rather than wasting the resource on known risks that can be managed other ways.
Starting March 15 everyone coming in had been required to self-isolate for two weeks, prior to the four-week lockdown we now have. At the moment, that precaution appears more than adequate to ensure they won't spread any disease they had on arrival.
Andre I accept the importance of community testing but surely stopping them coming in is paramount. On the AM show this morning there was talk of a private company in NZ capable of supplying test kits and has been trying to get the Government to take some interest for two weeks. Without any luck to date. We all know some people just don’t self isolate don’t we Andre. We know the Government has its protocols but maybe they should look outside of their bubble.
This private company, are they the ones in joe90's first comment in today's Open Mike? https://thestandard.org.nz/open-mike-30-03-2020/#comment-1696221
Also, when it comes to arseholes that repay the privilege of being allowed back in the midst of a pandemic by breaking self-isolation, there's other ways of dealing with them. Personally I'm not averse to the idea of just shooting them, but I accept I'm probably out on the fringes of public opinion on that one. There’s still no need to further privilege them by wasting limited testing resources on all of them for the sake of finding the very few that are both infected and antisocial enough to break self-isolation.
What would be the purpose of testing them? Returning citizens either have a satisfactory self-isolation plan or are carted off to a dedicated quarantine hotel for two weeks, so if they have the virus that will be revealed by the isolation period. It therefore makes no sense to waste much-needed test kits on those people rather than putting them to good use pinning down community transmission.
Sorry PM but those who are supposedly self isolating would think twice about breaking ranks if a phone call came through with a positive. Just because you and I say we’re going to do this properly doesn’t mean everybody will. It’s my point of view and I can’t see why it’s a wasted test where you would also have their contact number and be able to reinforce the message if a positive turns up rather than trying to chase them up after the fact when they didn’t self isolate properly and put the community at risk.
New View – you seem to think the test is infallible. As I understand, during the early stage of infection, the test shows negative, It is not infallible. Isolation and time is a more valid test – the isolation just has to be enforced.
You are correct. For all tests, there is a trade-off between sensitivity and specificity.
https://en.wikipedia.org/wiki/Sensitivity_and_specificity
No I don’t think the test is infallible’ I think it’s a big red light for those who might get a positive to be on super alert with their isolation. Those not displaying symptoms but positive might be tempted to push the isolation boundaries to the detriment of the community. If there is only a few hundred coming into the country on a daily basis wouldn’t you just test to be on the safe side and close one more door. Silly me for being overly careful.
Silly you. The isolation has to be enforced, and that is the only fail-proof test. Test kits which we are short of are needed more elsewhere. Obviously.
No 'safe side' at all as you conjecture.
As you will know it can’t be enforced in every case. I hope for our sakes it is enforced but can’t be. I personally know of returned friends that have isolated but only by chance. I won’t describe their complete circumstances but will say only that they live in a rural area and it was only their immediate family that reinforced the isolation. Other families may not be so lucky. The private company shown on the AM show could have supplied quick kits to the Government but they weren’t interested. Would have been fine for airport use even though slightly less accurate. I guess the Government knows best. 😔 🤪
Yes, they do and they made the right decision IMHO.
Yes it’s just your opinion as I have mine. You don’t explain why you think the Government have got this decision right.
Because it is a different type of test than the standard PCR-based one.
But don’t take my word for it, as you don’t know me, take the word of Dr Siouxsie Wiles: https://thespinoff.co.nz/science/31-03-2020/covid-19-what-difference-can-the-new-fast-turnaround-blood-tests-make/
I think that GPs are now testing, or getting tested, the people they think most likely to be Covid-19 positive. They need to be selective because the labs don't have the resources to test everyone. Testing of a sample of the general population should indicate the extent of community transmission, and likely hot spots.
When I had a phone consultation with a GP last Monday, I got that impression. I have a scratchy throat – more likely strep throat than the virus. She prescribed antibiotics.
I said I had been doing social/physical distancing as much as possible for the last few weeks, and hadn't had close contact with anyone in that period.
The GP said to self-isolate & stay away from other people just in case it's Covid-19. She said she wasn't going to get me tested for the virus – I don't have a fever or runny nose and feel fine. Also she said I'm a healthy 70 yr old without any underlying condition.
I haven't been out of my flat since then, except to put out rubbish & check the mailbox.
Aren't facts amazing – I don't why we bother with fiction:
Virus Wars – MRC LMB www2.mrc-lmb.cam.ac.uk › viruswars › viruses
www2.mrc-lmb.cam.ac.uk › viruswars › viruses
Every day you breathe in over 100,000,000 viruses. … Each antibody producing cell can produce 2000 antibody molecules per second. … by our white blood cells and are a major part of the body's response to combatting a viral infection.
For those who want all the nitty-gritty, in academic-speak (and it has coloured pics which make it easier to comprehend).
https://onlinelibrary.wiley.com/doi/10.1002/jmv.25685 Journal of Medical Virology (Free Access!)
Coronavirus infections and immune responses
(It includes quite a list a list of receptors – I think we should bring the Welcome doormat inside, myself. Then it goes on to Type 1 interferons, dendritic cells and defensins. This is the perfect link to swot up on so you can bat everyone else's mere opinions, with, seemingly, perfect authority!)
Evolution is relentless. The more one species exploits its environment the more other species will respond, die or exploit.
The fastest are microbial, fungi etc.
CVD19 just struck it lucky in evolutionary Lotto
The space humans have been taking over the planet is obviously unsustainable.
As we become extinct Ther are plenty of organisms available to exploit what is left.
WE ARE IN THIS ALL TOGETHER, (regardless of what boris trump and/or donald johnson have to say about it.
Evolution will out.
My grandmother walked with a brace her whole life because of polio. I got a shot.
i got rubella (german measles), I was kept away from school for a month, because everyone in NZ knew someone who knew someone who had had a child who had a birth defect because their mother had contracted it during pregnancy. Mothers kept us home because it could have been them, or us.
My kids got chicken pox literally the week before the vaccine became available – they might have shingles when they are old (but there is a vaccine).
The only reason we have anti-vaxxers is because we have forgotten all this – these are family stories we need to tell our kids, grandkids, etc so that no one forgets
I, for one, have absolutely no real interest in dying for tourism
We have had avalanche after avalanche of Tourism in recent years, the Faeces from which has been strewn freely the length and breadth of the country.
Somebody must have made $millions. But why were they allowed to bring huge overloads of visitors ?
When the Governments of the past 40 years should have been building State houses ! By now, the words "LandLord" and "Homeless" should have vanished from Aotearoa.
It would be nice if Kiwis who live here get to see their own Nation. At realistic Cost.