 Guest post – is it safe to lower the lockdown level?
Guest post – is it safe to lower the lockdown level?
Written By:
Guest post - Date published:
10:41 am, April 20th, 2020 - 58 comments
Categories: Deep stuff, health and safety, Politics -
Tags: covid-19, Covid19
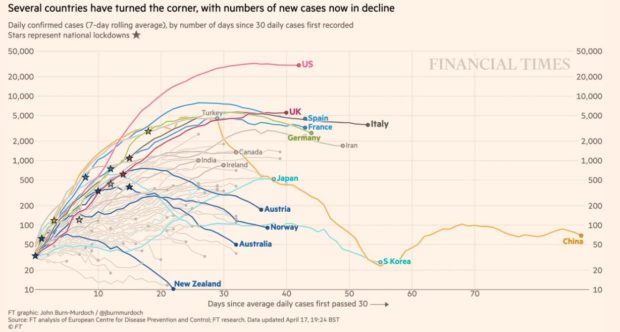
Taken from a comment by Karl Sinclair.
Question: Is it safe to move now from level 4 to progressively lower levels?
Recommendation: Do not move to level 3 until we have:
- Robust testing strategies and capabilities in place to trace asymptomatic cases within our essential worker populations etc.
- The ability to protect the vulnerable
- Reviewed the effect on other countries moves to lower levels, such as Denmark, to gain their lessons learned.
Put it like this, would you fly in a plane that had this many design unknowns and lack of ground support?
PROBLEM STATEMENT:
COVID 19 is making it difficult for country to return to “normal life”. Safety levels have been put in place to help us return to normal. The effects of these levels are both positive and negative. The positives being the increase in lives saved, improved health outcomes, and an economy recovering quicker. The negatives (are effectively the opposite) can be seen in terms of loss of income, economic decline, and associated poor health outcomes (even loss of life) if people cannot get back to work.
Some might say this is a “wicked problem”, a balancing act, that will require precision and timing.
Key questions to ask before moving to level 3:
- Do we have the capability to move down levels and provide sustained protection to the vulnerable while we wait for a vaccine (if one comes at all?)?
- Do we have robust and sufficient COVID testing capabilities and PPE (to allow people back to work and ensure virus free health care providers)
- Are NZs testing strategies (essential workers targeted) robust enough to catch the asymptomatic spreaders?
- Do we have robust tracking and data base and data reporting capabilities?
- Do we have sufficient medical and elderly care capabilities (people, training and equipment)?
- Do we know enough about the virus to mitigate risk?
- Should NZ hold at level 4 to learn from other countries strategies (Denmark just reduced its level to allow school children back to school, what was the effect)?
- What is the confidence of eliminating the virus completely within NZ?
- Do we have the right criteria within the levels?
These questions will remain relevant to New Zealand as at some point we will need to get back to work and open our boarders. Essentially we have the moral imperative (momentum) to develop and invest in a capability to protect us from pandemics now and into the future. We need to find solutions.
Dr Chris Smith, consultant clinical virologist at Cambridge University in the UK said recently on Radio New Zealand: “this will be very difficult to eliminate Covid-19 completely from circulation in New Zealand when so many cases are believed to be asymptomatic”
THE IMPORTANCE OF QUALITY TESTING & REVIEWING OTHER COUNTRIES APPROACHES (before going over top of the trenches)
Sweden, Norway and Denmark may provide good comparison with New Zealand as population size/density, quality of health care and geography are to a degree similar (however, these countries are part of Europe, where an island nation). Other countries could be studied. The following data was taken from worldometer on the 19 April 2019 for all 3 Nordic countries:
- Sweden: Population 10.2 Million, 13,822 COVID positive, deaths 1,511, with 1,054 critical, deaths per million = 150.
- Denmark: Population 5.8 Million, 7242 COVID positive, deaths 346, with 76 critical, deaths per million = 60
- Norway Population 5.4 Million, 7069 COVID positive, deaths 164, with 63 critical, deaths per million = 30
Denmark and Norway have been seen to implement firmer restrictions than Sweden. Sweden may serve as an insight into how many would die or become critical if a “lighter” approach is taken by New Zealand (mimics a move to level 3 or 2). Can New Zealand sustain 1,054 critical patients or let alone 1,511 deaths that Sweden has? Comparing approach and consequent fatality and infection levels between Sweden, Denmark and Norway may help us to refine a strategy (taking into consideration the lag before the benefits of the measures are seen) as the latter two countries took a more strict approach.
An older exert from a web site called “The Local” on the 31st March 2020 compared the Danish, Norwegian and Swedish approaches.
An interesting comment from Swedish state epidemiologist Anders Tegnelll:
If Sweden’s health system is overwhelmed, then Denmark and Norway will feel their tougher policies were justified. But the real test of Sweden’s strategy will come later, when Denmark and Norway start to lift their lockdowns. Can they return to normal without the infection flaring up again? Will they be hit by a second wave this winter? Will any additional deaths Sweden sees over this Easter be the price it pays for having fewer over the coming years? “This is not a disease that you get rid of. And if you don’t get rid of it, what are you waiting for?” Tegnell said. “You can either wait for some kind of immunity to develop in your population, or you can wait for a vaccine. And the vaccine is, most likely, at least a year away.”
The current graph comparing the Nordic countries can be found here:
What exactly are the capabilities being put in place by these countries to keep the vulnerable safe? An alarming report dated April 20th 2020 from the Guardian discusses the lack of protection for the elderly in Sweden. Selected abridged quotes highlight:
Lena Einhorn, a virologist: “They have to admit that it’s a huge failure, since they have said the whole time that their main aim has been to protect the elderly,” she said. “But what is really strange is that they still do not acknowledge the likely route. They say it’s very unfortunate, that they are investigating, and that it’s a matter of the training personnel, but they will not acknowledge that presymptomatic or asymptomatic spread is a factor.”
the reason why Sweden has a much higher number of cases in care homes than in Norway and Finland is not because of the homes themselves, but because of Sweden’s decision to keep schools and kindergartens open, and not to shut restaurants or bars. “It’s not like it goes from one old age home to another. It comes in separately to all of these old age homes, so there’s no way it can be all be attributed to the personnel going in and working when they are sick. There’s a basic system fault in their recommendations. There’s no other explanation for it.”
“The worst thing is that it is us, the staff, who are taking the infection in to the elderly,” complained one nurse to Swedish public broadcaster SVT. “It’s unbelievable that more of them haven’t been infected. It’s a scandal.”
Although the above is just an exercise is New Zealands testing strategy going down Sweden’s path or is it more like Norways and Denmarks?
Numerous epidemiologists and scientists in New Zealand (and abroad noble prize winners) have been pressing for obtaining sufficient quality accurate test data to make informed decisions. Presume this also means sampling strategies and good data (not just random samples from selected supermarket chains but sentinel testing strategies) to ensure we improve our confidence in the data before changing levels. Various quotes:
- Otago University Professor and epidemiologist Sir David Skegg comment we will be playing “Russian roulette” with the health of New Zealanders if it makes a lockdown decision without first vastly improving rapid contact-tracing and collecting more information about Covid-19 in vulnerable communities. See
- Prof. M Baker – There appear to be gaps in the Government’s data on Covid-19 that must be filled before a decision is made on reducing the lockdown level, two top advisers say.
- Sir Peter Glucman has looked at how New Zealand could move from alert level 4 to alert level 2 as quickly as possible, however, it was mentioned in the article: “Given the inevitability of imperfect elimination, and given some probable level of asymptomatic and pre-symptomatic spread, it will be critical to have rapid and highly effective and high capacity contact tracing in place before relaxing restrictions.”
- Professor Paul Shaun Hendy, an expert on modelling how the coronavirus spreads says New Zealand’s alert level 4 lockdown should be continued for another two weeks to strengthen chances of eliminating Covid-19.
- Paul Romer Nobel Lareate in economics: quote “ He imagines health workers being tested at the start of a shift; the same would go for care workers, pharmacists, police officers and bus drivers. You might add teachers and restaurant workers. Romer wouldn’t bother testing people who already have symptoms: they should be presumed positive and immediately self-isolate. It’s the “asymptomatic spreaders” you need to identify, stopping them in their tracks. The logic underpinning the plan is clear: there will be no point in reopening shops, pubs and restaurants if people feel too scared to visit them. As virologist Prof Nicolas Locker puts it, “You can’t lift the lockdown as long as you are not testing massively.”….. Governments need to realise that what’s coming is not a decision about easing this or that rule of social distancing, but rather a massive political, industrial and collective drive unseen since the last war. It may well mean repurposing factories to mass-produce testing kits. At the very least, it should mean a dedicated cabinet minister for testing.,,,,,,,,,,,,This demands a huge shift by the UK government, which wasn’t even testing people coming out of hospital and going into social care until this week.
Also see Paul Romers tweet.
The twitter thread version of my plan:
— Paul Romer (@paulmromer) April 10, 2020
0. Stop testing people with symptoms. Presume positive and isolate.
Can we as a country honestly say New Zealand has the capability to protect our vulnerable and at the same time get our country back to work (move from level 4 down)? We might be lucky and have eliminated it, however, various experts say there is a high probability we won’t and at some point New Zealand will have to get back to work.
What can be gleaned from Paul Romer Nobel Lareates words above is that in the New Zealand context, we need to ensure a meaningful surveillance testing strategy and adapting new testing technology as it emerges (this appears to be what is happening in the USA). This testing can allow for creation of safe communities, workplaces, supply chains etc. It can also be used to protect the vulnerable by testing all people that work or deliver goods/services to care facilities before they enter.
For example, people can be tested before entering a workplace. Testing (if fit for purpose) will allow for the protection of the vulnerable such that it could buy time until a safe vaccine is developed and/or NZ is COVID free.
Testing (accuracy and quality still under review) to get the people back to work and protect the vulnerable being discussed in the USA and around the world include:
- Fast Antibody testing (catch asymptomatic)
- Fast COVID testing (proves you have it)
Building on Paul Romer Nobel Lareates ideas for NZ, its presumed essential workers level 4 and 3 who are the most likely transmission points could be tested. An example of the numbers involved in NZ is given below (a statistical subset of each work function could be taken if we do not have the capability).
- 8,100 Police frontline officers
- 58,206 enrolled nurses
- 13,883 registered active doctors
- 859 registered surgeons
- 62,000 Supermarket workers
- 2000 Career and 11,000 volunteer Fire Fighters
- ? Port workers
Think permutations and combinations of possible infection!!!!! Is astronomical the hiding place this virus can be in
Before we open schools we need to be cognisant of the numbers involved: Primary Pupils = 475,797, Secondary School Pupils = 286,886 and teachers = 70,000 Also there is approximately 60,000 pre-schoolers.
In addition to the above testing data needs, the risk attributes of virus listed below need to be determined to help develop a meaningful strategy:
- Immunity (does infection guarantee immunity, if so, for how long)
- Time infectious?
- Reactivation (like chicken pox you could reinfect people)
- Mutation (can the virus mutate and become more deadly)
- What’s the combined effects of flu, common cold with COVID 19
- How long does it take an individual to recover (long term effects and cost)
- Percentage of people susceptible that don’t have pre-existing conditions
- Time till development of a vaccine (if ever)
Further Questions:
- Could NZ Inc concentrate on developing safe facilities and capabilities (testing health care workers etc) for the vulnerable (elderly and or people with pre-existing comorbidities) going forward regardless? This would act as a safeguard or insurance policy (a controllable) if no vaccine or reliable anti body tests are found allowing schools and businesses to reopen.
- Is greater caution required before we move down a level given Japan and other countries are experiencing second waves of the virus.
- In terms of NZs technical advisory groups, have we ensured a wide enough expertise to cover off all areas from science, health, economics (designing strategy) all the way through to practical implementation (logistics and operations)? For example, MPI and NZDF will have good practical experience
Take care everyone, the world greatest ever game of whack a mole is about to begin.
Related Posts
58 comments on “Guest post – is it safe to lower the lockdown level? ”
- Comments are now closed
- Comments are now closed
Recent Comments
- Anne on
- Barfly on
- Visubversa to tWig on
- Michael Scott to tc on
- Anne on
- tWig on
- tWig on
- Michael Scott to Michael Scott on
- tc on
- Subliminal on
- Drowsy M. Kram to Reality on
- PsyclingLeft.Always to georgecom on
- SPC on
- SPC on
- Rodel to tsmithfield on
- SPC on
- georgecom to tsmithfield on
- PsyclingLeft.Always to joe90 on
- joe90 to PsyclingLeft.Always on
- Reality on
- PsyclingLeft.Always to joe90 on
- joe90 on
- joe90 on
- SPC to tsmithfield on
- Res Publica to ghostwhowalksnz on
- tsmithfield to JeremyB on
- Kay to tsmithfield on
- mpledger to tsmithfield on
- Reality on
- adam on
- Ad on
- joe90 on
- tsmithfield on
- tsmithfield to Barfly on
- I Feel Love to tsmithfield on
- Barfly to tsmithfield on
- tsmithfield on
Recent Posts
-
by mickysavage
-
by mickysavage
-
by mickysavage
-
by Guest post
-
by Mountain Tui
-
by mickysavage
-
by mickysavage
-
by lprent
-
by Mountain Tui
-
by Mountain Tui
-
by Mountain Tui
-
by weka
-
by Mountain Tui
-
by Mountain Tui
-
by mickysavage
-
by mickysavage
-
by Mountain Tui
-
by lprent
-
by Mountain Tui
-
by mickysavage
-
by lprent
-
by Guest post
-
by Guest post
-
by mickysavage
-
by mickysavage
- Stories of varying weight
More Than A FeildingBy David Slack5 hours ago
- Balancing External Security and the Economy
 New Zealand is again having to reconcile conflicting pressures from its military and its trade interests. Should we join Pillar Two of AUKUS and risk compromising our markets in China? For a century after New Zealand was founded in 1840, its external security arrangements and external economics arrangements were aligned. ...PunditBy Brian Easton17 hours ago
New Zealand is again having to reconcile conflicting pressures from its military and its trade interests. Should we join Pillar Two of AUKUS and risk compromising our markets in China? For a century after New Zealand was founded in 1840, its external security arrangements and external economics arrangements were aligned. ...PunditBy Brian Easton17 hours ago - Weekly Climate Wrap: The unravelling of the offsets
The KakaBy Bernard Hickey22 hours ago
- What makes us tick
 This morning the sky was bright.The birds, in their usual joyous bliss. Nature doesn’t seem to feel the heat of what might angst humans.Their calls are clear and beautiful.Just some random thoughts:MāoriPaul Goldsmith has announced his government will roll back the judiciary’s rulings on Māori Customary Marine Title, which recognises ...Mountain TuiBy Mountain Tui23 hours ago
This morning the sky was bright.The birds, in their usual joyous bliss. Nature doesn’t seem to feel the heat of what might angst humans.Their calls are clear and beautiful.Just some random thoughts:MāoriPaul Goldsmith has announced his government will roll back the judiciary’s rulings on Māori Customary Marine Title, which recognises ...Mountain TuiBy Mountain Tui23 hours ago - Foreshore and seabed 2.0
 In 2003, the Court of Appeal delivered its decision in Ngati Apa v Attorney-General, ruling that Māori customary title over the foreshore and seabed had not been universally extinguished, and that the Māori Land Court could determine claims and confirm title if the facts supported it. This kicked off the ...No Right TurnBy Idiot/Savant1 day ago
In 2003, the Court of Appeal delivered its decision in Ngati Apa v Attorney-General, ruling that Māori customary title over the foreshore and seabed had not been universally extinguished, and that the Māori Land Court could determine claims and confirm title if the facts supported it. This kicked off the ...No Right TurnBy Idiot/Savant1 day ago - Gordon Campbell on the Royal Commission report into abuse in care
 Earlier this week at Parliament, Labour leader Chris Hipkins was applauded for saying that the response to the final report of the Royal Commission of Inquiry into Abuse in Care had to be “bigger than politics.” True, but the fine words, apologies and “we hear you” messages will soon ring ...WerewolfBy lyndon1 day ago
Earlier this week at Parliament, Labour leader Chris Hipkins was applauded for saying that the response to the final report of the Royal Commission of Inquiry into Abuse in Care had to be “bigger than politics.” True, but the fine words, apologies and “we hear you” messages will soon ring ...WerewolfBy lyndon1 day ago - The Kākā’s Pick 'n' Mix for Friday, July 26
 TL;DR: In news breaking this morning:The Ministry of Education is cutting $2 billion from its school building programme so the National-ACT-NZ First Coalition Government has enough money to deliver tax cuts; The Government has quietly lowered its child poverty reduction targets to make them easier to achieve;Te Whatu Ora-Health NZ’s ...The KakaBy Bernard Hickey1 day ago
TL;DR: In news breaking this morning:The Ministry of Education is cutting $2 billion from its school building programme so the National-ACT-NZ First Coalition Government has enough money to deliver tax cuts; The Government has quietly lowered its child poverty reduction targets to make them easier to achieve;Te Whatu Ora-Health NZ’s ...The KakaBy Bernard Hickey1 day ago - Weekly Roundup 26-July-2024
 Kia ora. These are some stories that caught our eye this week – as always, feel free to share yours in the comments. Our header image this week (via Eke Panuku) shows the planned upgrade for the Karanga Plaza Tidal Swimming Steps. The week in Greater Auckland On ...Greater AucklandBy Greater Auckland1 day ago
Kia ora. These are some stories that caught our eye this week – as always, feel free to share yours in the comments. Our header image this week (via Eke Panuku) shows the planned upgrade for the Karanga Plaza Tidal Swimming Steps. The week in Greater Auckland On ...Greater AucklandBy Greater Auckland1 day ago - God what a relief
More Than A FeildingBy David Slack1 day ago
- Trust In Me
 Trust in me in all you doHave the faith I have in youLove will see us through, if only you trust in meWhy don't you, you trust me?In a week that saw the release of the 3,000 page Abuse in Care report Christopher Luxon was being asked about Boot Camps. ...Nick’s KōreroBy Nick Rockel1 day ago
Trust in me in all you doHave the faith I have in youLove will see us through, if only you trust in meWhy don't you, you trust me?In a week that saw the release of the 3,000 page Abuse in Care report Christopher Luxon was being asked about Boot Camps. ...Nick’s KōreroBy Nick Rockel1 day ago - The Hoon around the week to July 26
TL;DR: The podcast above of the weekly ‘hoon’ webinar for paying subscribers last night features co-hosts and talking about the Royal Commission Inquiry into Abuse in Care report released this week, and with:The Kākā’s climate correspondent on a UN push to not recognise carbon offset markets and ...The KakaBy Bernard Hickey1 day ago
- The Kākā’s Journal of Record for Friday, July 26
 TL;DR: As of 6:00 am on Friday, July 26, the top six announcements, speeches, reports and research around housing, climate and poverty in Aotearoa’s political economy in the last day are:Transport: Simeon Brown announced $802.9 million in funding for 18 new trains on the Wairarapa and Manawatū rail lines, which ...The KakaBy Bernard Hickey1 day ago
TL;DR: As of 6:00 am on Friday, July 26, the top six announcements, speeches, reports and research around housing, climate and poverty in Aotearoa’s political economy in the last day are:Transport: Simeon Brown announced $802.9 million in funding for 18 new trains on the Wairarapa and Manawatū rail lines, which ...The KakaBy Bernard Hickey1 day ago - Radical law changes needed to build road
 The northern expressway extension from Warkworth to Whangarei is likely to require radical changes to legislation if it is going to be built within the foreseeable future. The Government’s powers to purchase land, the planning process and current restrictions on road tolling are all going to need to be changed ...PolitikBy Richard Harman1 day ago
The northern expressway extension from Warkworth to Whangarei is likely to require radical changes to legislation if it is going to be built within the foreseeable future. The Government’s powers to purchase land, the planning process and current restrictions on road tolling are all going to need to be changed ...PolitikBy Richard Harman1 day ago - Skeptical Science New Research for Week #30 2024
 Open access notables Could an extremely cold central European winter such as 1963 happen again despite climate change?, Sippel et al., Weather and Climate Dynamics: Here, we first show based on multiple attribution methods that a winter of similar circulation conditions to 1963 would still lead to an extreme seasonal ...2 days ago
Open access notables Could an extremely cold central European winter such as 1963 happen again despite climate change?, Sippel et al., Weather and Climate Dynamics: Here, we first show based on multiple attribution methods that a winter of similar circulation conditions to 1963 would still lead to an extreme seasonal ...2 days ago - First they came for the Māori
Mountain TuiBy Mountain Tui2 days ago
- Join us for the weekly Hoon on YouTube Live
 Photo by Joshua J. Cotten on UnsplashWe’re back again after our mid-winter break. We’re still with the ‘new’ day of the week (Thursday rather than Friday) when we have our ‘hoon’ webinar with paying subscribers to The Kākā for an hour at 5 pm.Jump on this link on YouTube Livestream ...The KakaBy Bernard Hickey2 days ago
Photo by Joshua J. Cotten on UnsplashWe’re back again after our mid-winter break. We’re still with the ‘new’ day of the week (Thursday rather than Friday) when we have our ‘hoon’ webinar with paying subscribers to The Kākā for an hour at 5 pm.Jump on this link on YouTube Livestream ...The KakaBy Bernard Hickey2 days ago - Will the real PM Luxon please stand up?
Mountain TuiBy Mountain Tui2 days ago
- Will debt reduction trump abuse in care redress?
 Luxon speaks in Parliament yesterday about the Abuse in Care report. Photo: Hagen Hopkins/Getty ImagesTL;DR: The top six things I’ve noted around housing, climate and poverty in Aotearoa’s political economy today are:PM Christopher Luxon said yesterday in tabling the Abuse in Care report in Parliament he wanted to ‘do the ...The KakaBy Bernard Hickey2 days ago
Luxon speaks in Parliament yesterday about the Abuse in Care report. Photo: Hagen Hopkins/Getty ImagesTL;DR: The top six things I’ve noted around housing, climate and poverty in Aotearoa’s political economy today are:PM Christopher Luxon said yesterday in tabling the Abuse in Care report in Parliament he wanted to ‘do the ...The KakaBy Bernard Hickey2 days ago - Olywhites and Time Bandits
 About a decade ago I worked with a bloke called Steve. He was the grizzled veteran coder, a few years older than me, who knew where the bodies were buried - code wise. Despite his best efforts to be approachable and friendly he could be kind of gruff, through to ...Nick’s KōreroBy Nick Rockel2 days ago
About a decade ago I worked with a bloke called Steve. He was the grizzled veteran coder, a few years older than me, who knew where the bodies were buried - code wise. Despite his best efforts to be approachable and friendly he could be kind of gruff, through to ...Nick’s KōreroBy Nick Rockel2 days ago - Why were the 1930s so hot in North America?
 This is a re-post from Yale Climate Connections by Jeff Masters and Bob Henson Those who’ve trawled social media during heat waves have likely encountered a tidbit frequently used to brush aside human-caused climate change: Many U.S. states and cities had their single hottest temperature on record during the 1930s, setting incredible heat marks ...2 days ago
This is a re-post from Yale Climate Connections by Jeff Masters and Bob Henson Those who’ve trawled social media during heat waves have likely encountered a tidbit frequently used to brush aside human-caused climate change: Many U.S. states and cities had their single hottest temperature on record during the 1930s, setting incredible heat marks ...2 days ago - Throwback Thursday – Thinking about Expressways
 Some of the recent announcements from the government have reminded us of posts we’ve written in the past. Here’s one from early 2020. There were plenty of reactions to the government’s infrastructure announcement a few weeks ago which saw them fund a bunch of big roading projects. One of ...Greater AucklandBy Greater Auckland2 days ago
Some of the recent announcements from the government have reminded us of posts we’ve written in the past. Here’s one from early 2020. There were plenty of reactions to the government’s infrastructure announcement a few weeks ago which saw them fund a bunch of big roading projects. One of ...Greater AucklandBy Greater Auckland2 days ago - The Kākā’s Pick 'n' Mix for Thursday, July 25
 TL;DR: My pick of the top six links elsewhere around housing, climate and poverty in Aotearoa’s political economy in the last day or so to 7:00 am on Thursday, July 25 are:News: Why Electric Kiwi is closing to new customers - and why it matters RNZ’s Susan EdmundsScoop: Government drops ...The KakaBy Bernard Hickey2 days ago
TL;DR: My pick of the top six links elsewhere around housing, climate and poverty in Aotearoa’s political economy in the last day or so to 7:00 am on Thursday, July 25 are:News: Why Electric Kiwi is closing to new customers - and why it matters RNZ’s Susan EdmundsScoop: Government drops ...The KakaBy Bernard Hickey2 days ago - The Possum: Demon or Friend?
 Hi,I felt a small wet tongue snaking through one of the holes in my Crocs. It explored my big toe, darting down one side, then the other. “He’s looking for some toe cheese,” said the woman next to me, words that still haunt me to this day.Growing up in New ...David FarrierBy David Farrier2 days ago
Hi,I felt a small wet tongue snaking through one of the holes in my Crocs. It explored my big toe, darting down one side, then the other. “He’s looking for some toe cheese,” said the woman next to me, words that still haunt me to this day.Growing up in New ...David FarrierBy David Farrier2 days ago - Not a story
 Yesterday I happily quoted the Prime Minister without fact-checking him and sure enough, it turns out his numbers were all to hell. It’s not four kg of Royal Commission report, it’s fourteen.My friend and one-time colleague-in-comms Hazel Phillips gently alerted me to my error almost as soon as I’d hit ...More Than A FeildingBy David Slack2 days ago
Yesterday I happily quoted the Prime Minister without fact-checking him and sure enough, it turns out his numbers were all to hell. It’s not four kg of Royal Commission report, it’s fourteen.My friend and one-time colleague-in-comms Hazel Phillips gently alerted me to my error almost as soon as I’d hit ...More Than A FeildingBy David Slack2 days ago - The Kākā’s Journal of Record for Thursday, July 25
 TL;DR: As of 6:00 am on Thursday, July 25, the top six announcements, speeches, reports and research around housing, climate and poverty in Aotearoa’s political economy in the last day were:The Abuse in Care Royal Commission of Inquiry published its final report yesterday.PM Christopher Luxon and The Minister responsible for ...The KakaBy Bernard Hickey2 days ago
TL;DR: As of 6:00 am on Thursday, July 25, the top six announcements, speeches, reports and research around housing, climate and poverty in Aotearoa’s political economy in the last day were:The Abuse in Care Royal Commission of Inquiry published its final report yesterday.PM Christopher Luxon and The Minister responsible for ...The KakaBy Bernard Hickey2 days ago - A tougher line on “proactive release”?
 The Official Information Act has always been a battle between requesters seeking information, and governments seeking to control it. Information is power, so Ministers and government agencies want to manage what is released and when, for their own convenience, and legality and democracy be damned. Their most recent tactic for ...No Right TurnBy Idiot/Savant3 days ago
The Official Information Act has always been a battle between requesters seeking information, and governments seeking to control it. Information is power, so Ministers and government agencies want to manage what is released and when, for their own convenience, and legality and democracy be damned. Their most recent tactic for ...No Right TurnBy Idiot/Savant3 days ago - 'Let's build a motorway costing $100 million per km, before emissions costs'
 TL;DR: The top six things I’ve noted around housing, climate and poverty in Aotearoa’s political economy today are:Transport and Energy Minister Simeon Brown is accelerating plans to spend at least $10 billion through Public Private Partnerships (PPPs) to extend State Highway One as a four-lane ‘Expressway’ from Warkworth to Whangarei ...The KakaBy Bernard Hickey3 days ago
TL;DR: The top six things I’ve noted around housing, climate and poverty in Aotearoa’s political economy today are:Transport and Energy Minister Simeon Brown is accelerating plans to spend at least $10 billion through Public Private Partnerships (PPPs) to extend State Highway One as a four-lane ‘Expressway’ from Warkworth to Whangarei ...The KakaBy Bernard Hickey3 days ago - Lester's Prescription – Positive Bleeding.
 I live my life (woo-ooh-ooh)With no control in my destinyYea-yeah, yea-yeah (woo-ooh-ooh)I can bleed when I want to bleedSo come on, come on (woo-ooh-ooh)You can bleed when you want to bleedYea-yeah, come on (woo-ooh-ooh)Everybody bleed when they want to bleedCome on and bleedGovernments face tough challenges. Selling unpopular decisions to ...Nick’s KōreroBy Nick Rockel3 days ago
I live my life (woo-ooh-ooh)With no control in my destinyYea-yeah, yea-yeah (woo-ooh-ooh)I can bleed when I want to bleedSo come on, come on (woo-ooh-ooh)You can bleed when you want to bleedYea-yeah, come on (woo-ooh-ooh)Everybody bleed when they want to bleedCome on and bleedGovernments face tough challenges. Selling unpopular decisions to ...Nick’s KōreroBy Nick Rockel3 days ago - Casey Costello gaslights Labour in the House
Please note:To skip directly to the- parliamentary footage in the video, scroll to 1:21 To skip to audio please click on the headphone icon on the left hand side of the screenThis video / audio section is under development. ...Mountain TuiBy Mountain Tui3 days ago
- Why is the Texas grid in such bad shape?
 This is a re-post from the Climate Brink by Andrew Dessler Headline from 2021 The Texas grid, run by ERCOT, has had a rough few years. In 2021, winter storm Uri blacked out much of the state for several days. About a week ago, Hurricane Beryl knocked out ...3 days ago
This is a re-post from the Climate Brink by Andrew Dessler Headline from 2021 The Texas grid, run by ERCOT, has had a rough few years. In 2021, winter storm Uri blacked out much of the state for several days. About a week ago, Hurricane Beryl knocked out ...3 days ago - Gordon Campbell on a textbook case of spending waste by the Luxon government
 Given the crackdown on wasteful government spending, it behooves me to point to a high profile example of spending by the Luxon government that looks like a big, fat waste of time and money. I’m talking about the deployment of NZDF personnel to support the US-led coalition in the Red ...WerewolfBy lyndon3 days ago
Given the crackdown on wasteful government spending, it behooves me to point to a high profile example of spending by the Luxon government that looks like a big, fat waste of time and money. I’m talking about the deployment of NZDF personnel to support the US-led coalition in the Red ...WerewolfBy lyndon3 days ago - The Kākā’s Pick 'n' Mix for Wednesday, July 24
 TL;DR: My pick of the top six links elsewhere around housing, climate and poverty in Aotearoa’s political economy in the last day or so to 7:40 am on Wednesday, July 24 are:Deep Dive: Chipping away at the housing crisis, including my comments RNZ/Newsroom’s The DetailNews: Government softens on asset sales, ...The KakaBy Bernard Hickey3 days ago
TL;DR: My pick of the top six links elsewhere around housing, climate and poverty in Aotearoa’s political economy in the last day or so to 7:40 am on Wednesday, July 24 are:Deep Dive: Chipping away at the housing crisis, including my comments RNZ/Newsroom’s The DetailNews: Government softens on asset sales, ...The KakaBy Bernard Hickey3 days ago - LXR Takaanini
 As I reported about the city centre, Auckland’s rail network is also going through a difficult and disruptive period which is rapidly approaching a culmination, this will result in a significant upgrade to the whole network. Hallelujah. Also like the city centre this is an upgrade predicated on the City ...Greater AucklandBy Patrick Reynolds3 days ago
As I reported about the city centre, Auckland’s rail network is also going through a difficult and disruptive period which is rapidly approaching a culmination, this will result in a significant upgrade to the whole network. Hallelujah. Also like the city centre this is an upgrade predicated on the City ...Greater AucklandBy Patrick Reynolds3 days ago - Four kilograms of pain
 Today, a 4 kilogram report will be delivered to Parliament. We know this is what the report of the Royal Commission of Inquiry into Abuse in State and Faith-based Care weighs, because our Prime Minister told us so.Some reporter had blindsided him by asking a question about something done by ...More Than A FeildingBy David Slack3 days ago
Today, a 4 kilogram report will be delivered to Parliament. We know this is what the report of the Royal Commission of Inquiry into Abuse in State and Faith-based Care weighs, because our Prime Minister told us so.Some reporter had blindsided him by asking a question about something done by ...More Than A FeildingBy David Slack3 days ago - The Kākā’s Journal of Record for Wednesday, July 24
 TL;DR: As of 7:00 am on Wednesday, July 24, the top six announcements, speeches, reports and research around housing, climate and poverty in Aotearoa’s political economy in the last day are:Beehive: Transport Minister Simeon Brown announced plans to use PPPs to fund, build and run a four-lane expressway between Auckland ...The KakaBy Bernard Hickey3 days ago
TL;DR: As of 7:00 am on Wednesday, July 24, the top six announcements, speeches, reports and research around housing, climate and poverty in Aotearoa’s political economy in the last day are:Beehive: Transport Minister Simeon Brown announced plans to use PPPs to fund, build and run a four-lane expressway between Auckland ...The KakaBy Bernard Hickey3 days ago - Luxon gets caught out
 NewstalkZB host Mike Hosking, who can usually be relied on to give Prime Minister Christopher Luxon an easy run, did not do so yesterday when he interviewed him about the HealthNZ deficit. Luxon is trying to use a deficit reported last year by HealthNZ as yet another example of the ...PolitikBy Richard Harman3 days ago
NewstalkZB host Mike Hosking, who can usually be relied on to give Prime Minister Christopher Luxon an easy run, did not do so yesterday when he interviewed him about the HealthNZ deficit. Luxon is trying to use a deficit reported last year by HealthNZ as yet another example of the ...PolitikBy Richard Harman3 days ago - A worrying sign
 Back in January a StatsNZ employee gave a speech at Rātana on behalf of tangata whenua in which he insulted and criticised the government. The speech clearly violated the principle of a neutral public service, and StatsNZ started an investigation. Part of that was getting an external consultant to examine ...No Right TurnBy Idiot/Savant4 days ago
Back in January a StatsNZ employee gave a speech at Rātana on behalf of tangata whenua in which he insulted and criticised the government. The speech clearly violated the principle of a neutral public service, and StatsNZ started an investigation. Part of that was getting an external consultant to examine ...No Right TurnBy Idiot/Savant4 days ago - Are we fine with 47.9% home-ownership by 2048?
 Renting for life: Shared ownership initiatives are unlikely to slow the slide in home ownership by much. Photo: Lynn Grieveson / The KākāTL;DR: The top six things I’ve noted around housing, climate and poverty in Aotearoa’s political economy today are:A Deloitte report for Westpac has projected Aotearoa’s home-ownership rate will ...The KakaBy Bernard Hickey4 days ago
Renting for life: Shared ownership initiatives are unlikely to slow the slide in home ownership by much. Photo: Lynn Grieveson / The KākāTL;DR: The top six things I’ve noted around housing, climate and poverty in Aotearoa’s political economy today are:A Deloitte report for Westpac has projected Aotearoa’s home-ownership rate will ...The KakaBy Bernard Hickey4 days ago - Let's Win This
 You're broken down and tiredOf living life on a merry go roundAnd you can't find the fighterBut I see it in you so we gonna walk it outAnd move mountainsWe gonna walk it outAnd move mountainsAnd I'll rise upI'll rise like the dayI'll rise upI'll rise unafraidI'll rise upAnd I'll ...Nick’s KōreroBy Nick Rockel4 days ago
You're broken down and tiredOf living life on a merry go roundAnd you can't find the fighterBut I see it in you so we gonna walk it outAnd move mountainsWe gonna walk it outAnd move mountainsAnd I'll rise upI'll rise like the dayI'll rise upI'll rise unafraidI'll rise upAnd I'll ...Nick’s KōreroBy Nick Rockel4 days ago - Waimahara: The Singing Spirit of Water
 There’s been a change in Myers Park. Down the steps from St. Kevin’s Arcade, past the grassy slopes, the children’s playground, the benches and that goat statue, there has been a transformation. The underpass for Mayoral Drive has gone from a barren, grey, concrete tunnel, to a place that thrums ...Greater AucklandBy Connor Sharp4 days ago
There’s been a change in Myers Park. Down the steps from St. Kevin’s Arcade, past the grassy slopes, the children’s playground, the benches and that goat statue, there has been a transformation. The underpass for Mayoral Drive has gone from a barren, grey, concrete tunnel, to a place that thrums ...Greater AucklandBy Connor Sharp4 days ago - A major milestone: Global climate pollution may have just peaked
 This is a re-post from Yale Climate Connections Global society may have finally slammed on the brakes for climate-warming pollution released by human fossil fuel combustion. According to the Carbon Monitor Project, the total global climate pollution released between February and May 2024 declined slightly from the amount released during the same ...4 days ago
This is a re-post from Yale Climate Connections Global society may have finally slammed on the brakes for climate-warming pollution released by human fossil fuel combustion. According to the Carbon Monitor Project, the total global climate pollution released between February and May 2024 declined slightly from the amount released during the same ...4 days ago - The Kākā’s Pick 'n' Mix for Tuesday, July 23
 TL;DR: My pick of the top six links elsewhere around housing, climate and poverty in Aotearoa’s political economy in the last day or so to 7:00 am on Tuesday, July 23 are:Deep Dive: Penlink: where tolling rhetoric meets reality BusinessDesk-$$$’s Oliver LewisScoop: Te Pūkenga plans for regional polytechs leak out ...The KakaBy Bernard Hickey4 days ago
TL;DR: My pick of the top six links elsewhere around housing, climate and poverty in Aotearoa’s political economy in the last day or so to 7:00 am on Tuesday, July 23 are:Deep Dive: Penlink: where tolling rhetoric meets reality BusinessDesk-$$$’s Oliver LewisScoop: Te Pūkenga plans for regional polytechs leak out ...The KakaBy Bernard Hickey4 days ago - The Kākā’s Journal of Record for Tuesday, July 23
 TL;DR: As of 6:00 am on Tuesday, July 23, the top six announcements, speeches, reports and research around housing, climate and poverty in Aotearoa’s political economy in the last day are:Health: Shane Reti announced the Board of Te Whatu Ora- Health New Zealand was being replaced with Commissioner Lester Levy ...The KakaBy Bernard Hickey4 days ago
TL;DR: As of 6:00 am on Tuesday, July 23, the top six announcements, speeches, reports and research around housing, climate and poverty in Aotearoa’s political economy in the last day are:Health: Shane Reti announced the Board of Te Whatu Ora- Health New Zealand was being replaced with Commissioner Lester Levy ...The KakaBy Bernard Hickey4 days ago - HealthNZ and Luxon at cross purposes over budget blowout
 Health NZ warned the Government at the end of March that it was running over Budget. But the reasons it gave were very different to those offered by the Prime Minister yesterday. Prime Minister Christopher Luxon blamed the “botched merger” of the 20 District Health Boards (DHBs) to create Health ...PolitikBy Richard Harman4 days ago
Health NZ warned the Government at the end of March that it was running over Budget. But the reasons it gave were very different to those offered by the Prime Minister yesterday. Prime Minister Christopher Luxon blamed the “botched merger” of the 20 District Health Boards (DHBs) to create Health ...PolitikBy Richard Harman4 days ago - 2500-3000 more healthcare staff expected to be fired, as Shane Reti blames Labour for a budget defic...
 Long ReadKey Summary: Although National increased the health budget by $1.4 billion in May, they used an old funding model to project health system costs, and never bothered to update their pre-election numbers. They were told during the Health Select Committees earlier in the year their budget amount was deficient, ...Mountain TuiBy Mountain Tui4 days ago
Long ReadKey Summary: Although National increased the health budget by $1.4 billion in May, they used an old funding model to project health system costs, and never bothered to update their pre-election numbers. They were told during the Health Select Committees earlier in the year their budget amount was deficient, ...Mountain TuiBy Mountain Tui4 days ago - Might Kamala Harris be about to get a 'stardust' moment like Jacinda Ardern?
 As a momentous, historic weekend in US politics unfolded, analysts and commentators grasped for precedents and comparisons to help explain the significance and power of the choice Joe Biden had made. The 46th president had swept the Democratic party’s primaries but just over 100 days from the election had chosen ...PunditBy Tim Watkin5 days ago
As a momentous, historic weekend in US politics unfolded, analysts and commentators grasped for precedents and comparisons to help explain the significance and power of the choice Joe Biden had made. The 46th president had swept the Democratic party’s primaries but just over 100 days from the election had chosen ...PunditBy Tim Watkin5 days ago - Solutions Interview: Steven Hail on MMT & ecological economics
TL;DR: I’m casting around for new ideas and ways of thinking about Aotearoa’s political economy to find a few solutions to our cascading and self-reinforcing housing, poverty and climate crises.Associate Professor runs an online masters degree in the economics of sustainability at Torrens University in Australia and is organising ...The KakaBy Steven Hail5 days ago
- Reported back
 The Finance and Expenditure Committee has reported back on National's Local Government (Water Services Preliminary Arrangements) Bill. The bill sets up water for privatisation, and was introduced under urgency, then rammed through select committee with no time even for local councils to make a proper submission. Naturally, national's select committee ...No Right TurnBy Idiot/Savant5 days ago
The Finance and Expenditure Committee has reported back on National's Local Government (Water Services Preliminary Arrangements) Bill. The bill sets up water for privatisation, and was introduced under urgency, then rammed through select committee with no time even for local councils to make a proper submission. Naturally, national's select committee ...No Right TurnBy Idiot/Savant5 days ago - Vandrad the Viking, Christopher Coombes, and Literary Archaeology
 Some years ago, I bought a book at Dunedin’s Regent Booksale for $1.50. As one does. Vandrad the Viking (1898), by J. Storer Clouston, is an obscure book these days – I cannot find a proper online review – but soon it was sitting on my shelf, gathering dust alongside ...A Phuulish FellowBy strda2215 days ago
Some years ago, I bought a book at Dunedin’s Regent Booksale for $1.50. As one does. Vandrad the Viking (1898), by J. Storer Clouston, is an obscure book these days – I cannot find a proper online review – but soon it was sitting on my shelf, gathering dust alongside ...A Phuulish FellowBy strda2215 days ago - Gordon Campbell On The Biden Withdrawal
 History is not on the side of the centre-left, when Democratic presidents fall behind in the polls and choose not to run for re-election. On both previous occasions in the past 75 years (Harry Truman in 1952, Lyndon Johnson in 1968) the Democrats proceeded to then lose the White House ...WerewolfBy lyndon5 days ago
History is not on the side of the centre-left, when Democratic presidents fall behind in the polls and choose not to run for re-election. On both previous occasions in the past 75 years (Harry Truman in 1952, Lyndon Johnson in 1968) the Democrats proceeded to then lose the White House ...WerewolfBy lyndon5 days ago - Joe Biden's withdrawal puts the spotlight back on Kamala and the USA's complicated relatio...
 This is a free articleCoverageThis morning, US President Joe Biden announced his withdrawal from the Presidential race. And that is genuinely newsworthy. Thanks for your service, President Biden, and all the best to you and yours.However, the media in New Zealand, particularly the 1News nightly bulletin, has been breathlessly covering ...Mountain TuiBy Mountain Tui5 days ago
This is a free articleCoverageThis morning, US President Joe Biden announced his withdrawal from the Presidential race. And that is genuinely newsworthy. Thanks for your service, President Biden, and all the best to you and yours.However, the media in New Zealand, particularly the 1News nightly bulletin, has been breathlessly covering ...Mountain TuiBy Mountain Tui5 days ago - Why we have to challenge our national fiscal assumptions
 A homeless person’s camp beside a blocked-off slipped damage walkway in Freeman’s Bay: we are chasing our tail on our worsening and inter-related housing, poverty and climate crises. Photo: Photo: Lynn Grieveson / The KākāTL;DR: The top six things I’ve noted around housing, climate and poverty in Aotearoa’s political economy ...The KakaBy Bernard Hickey5 days ago
A homeless person’s camp beside a blocked-off slipped damage walkway in Freeman’s Bay: we are chasing our tail on our worsening and inter-related housing, poverty and climate crises. Photo: Photo: Lynn Grieveson / The KākāTL;DR: The top six things I’ve noted around housing, climate and poverty in Aotearoa’s political economy ...The KakaBy Bernard Hickey5 days ago - Existential Crisis and Damaged Brains
 What has happened to it all?Crazy, some'd sayWhere is the life that I recognise?(Gone away)But I won't cry for yesterdayThere's an ordinary worldSomehow I have to findAnd as I try to make my wayTo the ordinary worldYesterday morning began as many others - what to write about today? I began ...Nick’s KōreroBy Nick Rockel5 days ago
What has happened to it all?Crazy, some'd sayWhere is the life that I recognise?(Gone away)But I won't cry for yesterdayThere's an ordinary worldSomehow I have to findAnd as I try to make my wayTo the ordinary worldYesterday morning began as many others - what to write about today? I began ...Nick’s KōreroBy Nick Rockel5 days ago - A speed limit is not a target, and yet…
 This is a guest post from longtime supporter Mr Plod, whose previous contributions include a proposal that Hamilton become New Zealand’s capital city, and that we should switch which side of the road we drive on. A recent Newsroom article, “Back to school for the Govt’s new speed limit policy“, ...Greater AucklandBy Guest Post5 days ago
This is a guest post from longtime supporter Mr Plod, whose previous contributions include a proposal that Hamilton become New Zealand’s capital city, and that we should switch which side of the road we drive on. A recent Newsroom article, “Back to school for the Govt’s new speed limit policy“, ...Greater AucklandBy Guest Post5 days ago - The Kākā’s Pick 'n' Mix for Monday, July 22
 TL;DR: My pick of the top six links elsewhere around housing, climate and poverty in Aotearoa’s political economy in the last day or so to 7:00 am on Monday, July 22 are:Today’s Must Read: Father and son live in a tent, and have done for four years, in a million ...The KakaBy Bernard Hickey5 days ago
TL;DR: My pick of the top six links elsewhere around housing, climate and poverty in Aotearoa’s political economy in the last day or so to 7:00 am on Monday, July 22 are:Today’s Must Read: Father and son live in a tent, and have done for four years, in a million ...The KakaBy Bernard Hickey5 days ago - The Kākā’s Journal of Record for Monday, July 22
 TL;DR: As of 7:00 am on Monday, July 22, the top six announcements, speeches, reports and research around housing, climate and poverty in Aotearoa’s political economy in the last day are:US President Joe Biden announced via X this morning he would not stand for a second term.Multinational professional services firm ...The KakaBy Bernard Hickey5 days ago
TL;DR: As of 7:00 am on Monday, July 22, the top six announcements, speeches, reports and research around housing, climate and poverty in Aotearoa’s political economy in the last day are:US President Joe Biden announced via X this morning he would not stand for a second term.Multinational professional services firm ...The KakaBy Bernard Hickey5 days ago - 2024 SkS Weekly Climate Change & Global Warming News Roundup #29
 A listing of 32 news and opinion articles we found interesting and shared on social media during the past week: Sun, July 14, 2024 thru Sat, July 20, 2024. Story of the week As reflected by preponderance of coverage, our Story of the Week is Project 2025. Until now traveling ...6 days ago
A listing of 32 news and opinion articles we found interesting and shared on social media during the past week: Sun, July 14, 2024 thru Sat, July 20, 2024. Story of the week As reflected by preponderance of coverage, our Story of the Week is Project 2025. Until now traveling ...6 days ago - I'd like to share what I did this weekend
Mountain TuiBy Mountain Tui6 days ago
- For the children – Why mere sentiment can be a misleading force in our lives, and lead to unex...
 National: The Party of ‘Law and Order’ IntroductionThis weekend, the Government formally kicked off one of their flagship policy programs: a military style boot camp that New Zealand has experimented with over the past 50 years. Cartoon credit: Guy BodyIt’s very popular with the National Party’s Law and Order image, ...Mountain TuiBy Mountain Tui6 days ago
National: The Party of ‘Law and Order’ IntroductionThis weekend, the Government formally kicked off one of their flagship policy programs: a military style boot camp that New Zealand has experimented with over the past 50 years. Cartoon credit: Guy BodyIt’s very popular with the National Party’s Law and Order image, ...Mountain TuiBy Mountain Tui6 days ago - A friend in uncertain times
 Day one of the solo leg of my long journey home begins with my favourite sound: footfalls in an empty street. 5.00 am and it’s already light and already too warm, almost.If I can make the train that leaves Budapest later this hour I could be in Belgrade by nightfall; ...More Than A FeildingBy David Slack6 days ago
Day one of the solo leg of my long journey home begins with my favourite sound: footfalls in an empty street. 5.00 am and it’s already light and already too warm, almost.If I can make the train that leaves Budapest later this hour I could be in Belgrade by nightfall; ...More Than A FeildingBy David Slack6 days ago - The Chaotic World of Male Diet Influencers
 Hi,We’ll get to the horrific world of male diet influencers (AKA Beefy Boys) shortly, but first you will be glad to know that since I sent out the Webworm explaining why the assassination attempt on Donald Trump was not a false flag operation, I’ve heard from a load of people ...David FarrierBy David Farrier6 days ago
Hi,We’ll get to the horrific world of male diet influencers (AKA Beefy Boys) shortly, but first you will be glad to know that since I sent out the Webworm explaining why the assassination attempt on Donald Trump was not a false flag operation, I’ve heard from a load of people ...David FarrierBy David Farrier6 days ago - It's Starting To Look A Lot Like… Y2K
 Do you remember Y2K, the threat that hung over humanity in the closing days of the twentieth century? Horror scenarios of planes falling from the sky, electronic payments failing and ATMs refusing to dispense cash. As for your VCR following instructions and recording your favourite show - forget about it.All ...Nick’s KōreroBy Nick Rockel1 week ago
Do you remember Y2K, the threat that hung over humanity in the closing days of the twentieth century? Horror scenarios of planes falling from the sky, electronic payments failing and ATMs refusing to dispense cash. As for your VCR following instructions and recording your favourite show - forget about it.All ...Nick’s KōreroBy Nick Rockel1 week ago - Bernard’s Saturday Soliloquy for the week to July 20
 Climate Change Minister Simon Watts being questioned by The Kākā’s Bernard Hickey.TL;DR: My top six things to note around housing, climate and poverty in Aotearoa’s political economy in the week to July 20 were:1. A strategy that fails Zero Carbon Act & Paris targetsThe National-ACT-NZ First Coalition Government finally unveiled ...The KakaBy Bernard Hickey1 week ago
Climate Change Minister Simon Watts being questioned by The Kākā’s Bernard Hickey.TL;DR: My top six things to note around housing, climate and poverty in Aotearoa’s political economy in the week to July 20 were:1. A strategy that fails Zero Carbon Act & Paris targetsThe National-ACT-NZ First Coalition Government finally unveiled ...The KakaBy Bernard Hickey1 week ago - Pharmac Director, Climate Change Commissioner, Health NZ Directors – The latest to quit this m...
 Summary:As New Zealand loses at least 12 leaders in the public service space of health, climate, and pharmaceuticals, this month alone, directly in response to the Government’s policies and budget choices, what lies ahead may be darker than it appears. Tui examines some of those departures and draws a long ...Mountain TuiBy Mountain Tui1 week ago
Summary:As New Zealand loses at least 12 leaders in the public service space of health, climate, and pharmaceuticals, this month alone, directly in response to the Government’s policies and budget choices, what lies ahead may be darker than it appears. Tui examines some of those departures and draws a long ...Mountain TuiBy Mountain Tui1 week ago - Flooding Housing Policy
 The Minister of Housing’s ambition is to reduce markedly the ratio of house prices to household incomes. If his strategy works it would transform the housing market, dramatically changing the prospects of housing as an investment.Leaving aside the Minister’s metaphor of ‘flooding the market’ I do not see how the ...PunditBy Brian Easton1 week ago
The Minister of Housing’s ambition is to reduce markedly the ratio of house prices to household incomes. If his strategy works it would transform the housing market, dramatically changing the prospects of housing as an investment.Leaving aside the Minister’s metaphor of ‘flooding the market’ I do not see how the ...PunditBy Brian Easton1 week ago - A Voyage Among the Vandals: Accepted (Again!)
 As previously noted, my historical fantasy piece, set in the fifth-century Mediterranean, was accepted for a Pirate Horror anthology, only for the anthology to later fall through. But in a good bit of news, it turned out that the story could indeed be re-marketed as sword and sorcery. As of ...A Phuulish FellowBy strda2211 week ago
As previously noted, my historical fantasy piece, set in the fifth-century Mediterranean, was accepted for a Pirate Horror anthology, only for the anthology to later fall through. But in a good bit of news, it turned out that the story could indeed be re-marketed as sword and sorcery. As of ...A Phuulish FellowBy strda2211 week ago - The Kākā's Chorus for Friday, July 19
 An employee of tobacco company Philip Morris International demonstrates a heated tobacco device. Photo: Getty ImagesTL;DR: The top six things I’ve noted around housing, climate and poverty in Aotearoa’s political economy on Friday, July 19 are:At a time when the Coalition Government is cutting spending on health, infrastructure, education, housing ...The KakaBy Bernard Hickey1 week ago
An employee of tobacco company Philip Morris International demonstrates a heated tobacco device. Photo: Getty ImagesTL;DR: The top six things I’ve noted around housing, climate and poverty in Aotearoa’s political economy on Friday, July 19 are:At a time when the Coalition Government is cutting spending on health, infrastructure, education, housing ...The KakaBy Bernard Hickey1 week ago - The Kākā’s Pick 'n' Mix for Friday, July 19
 TL;DR: My pick of the top six links elsewhere around housing, climate and poverty in Aotearoa’s political economy in the last day or so to 8:30 am on Friday, July 19 are:Scoop: NZ First Minister Casey Costello orders 50% cut to excise tax on heated tobacco products. The minister has ...The KakaBy Bernard Hickey1 week ago
TL;DR: My pick of the top six links elsewhere around housing, climate and poverty in Aotearoa’s political economy in the last day or so to 8:30 am on Friday, July 19 are:Scoop: NZ First Minister Casey Costello orders 50% cut to excise tax on heated tobacco products. The minister has ...The KakaBy Bernard Hickey1 week ago - Weekly Roundup 19-July-2024
 Kia ora, it’s time for another Friday roundup, in which we pull together some of the links and stories that caught our eye this week. Feel free to add more in the comments! Our header image this week shows a foggy day in Auckland town, captured by Patrick Reynolds. ...Greater AucklandBy Greater Auckland1 week ago
Kia ora, it’s time for another Friday roundup, in which we pull together some of the links and stories that caught our eye this week. Feel free to add more in the comments! Our header image this week shows a foggy day in Auckland town, captured by Patrick Reynolds. ...Greater AucklandBy Greater Auckland1 week ago - Weekly Climate Wrap: A market-led plan for failure
TL;DR : Here’s the top six items climate news for Aotearoa this week, as selected by Bernard Hickey and The Kākā’s climate correspondent Cathrine Dyer. A discussion recorded yesterday is in the video above and the audio of that sent onto the podcast feed.The Government released its draft Emissions Reduction ...The KakaBy Bernard Hickey1 week ago
- Tobacco First
 Save some money, get rich and old, bring it back to Tobacco Road.Bring that dynamite and a crane, blow it up, start all over again.Roll up. Roll up. Or tailor made, if you prefer...Whether you’re selling ciggies, digging for gold, catching dolphins in your nets, or encouraging folks to flutter ...Nick’s KōreroBy Nick Rockel1 week ago
Save some money, get rich and old, bring it back to Tobacco Road.Bring that dynamite and a crane, blow it up, start all over again.Roll up. Roll up. Or tailor made, if you prefer...Whether you’re selling ciggies, digging for gold, catching dolphins in your nets, or encouraging folks to flutter ...Nick’s KōreroBy Nick Rockel1 week ago - Trump’s Adopted Son.
 Waiting In The Wings: For truly, if Trump is America’s un-assassinated Caesar, then J.D. Vance is America’s Octavian, the Republic’s youthful undertaker – and its first Emperor.DONALD TRUMP’S SELECTION of James D. Vance as his running-mate bodes ill for the American republic. A fervent supporter of Viktor Orban, the “illiberal” prime ...1 week ago
Waiting In The Wings: For truly, if Trump is America’s un-assassinated Caesar, then J.D. Vance is America’s Octavian, the Republic’s youthful undertaker – and its first Emperor.DONALD TRUMP’S SELECTION of James D. Vance as his running-mate bodes ill for the American republic. A fervent supporter of Viktor Orban, the “illiberal” prime ...1 week ago - The Kākā’s Journal of Record for Friday, July 19
 TL;DR: As of 6:00 am on Friday, July 19, the top six announcements, speeches, reports and research around housing, climate and poverty in Aotearoa’s political economy in the last day are:The PSA announced the Employment Relations Authority (ERA) had ruled in the PSA’s favour in its case against the Ministry ...The KakaBy Bernard Hickey1 week ago
TL;DR: As of 6:00 am on Friday, July 19, the top six announcements, speeches, reports and research around housing, climate and poverty in Aotearoa’s political economy in the last day are:The PSA announced the Employment Relations Authority (ERA) had ruled in the PSA’s favour in its case against the Ministry ...The KakaBy Bernard Hickey1 week ago - The Hoon around the week to July 19
TL;DR: The podcast above of the weekly ‘hoon’ webinar for paying subscribers last night features co-hosts and talking with:The Kākā’s climate correspondent talking about the National-ACT-NZ First Government’s release of its first Emissions Reduction Plan;University of Otago Foreign Relations Professor and special guest Dr Karin von ...The KakaBy Bernard Hickey1 week ago
- Skeptical Science New Research for Week #29 2024
 Open access notables Improving global temperature datasets to better account for non-uniform warming, Calvert, Quarterly Journal of the Royal Meteorological Society: To better account for spatial non-uniform trends in warming, a new GITD [global instrumental temperature dataset] was created that used maximum likelihood estimation (MLE) to combine the land surface ...1 week ago
Open access notables Improving global temperature datasets to better account for non-uniform warming, Calvert, Quarterly Journal of the Royal Meteorological Society: To better account for spatial non-uniform trends in warming, a new GITD [global instrumental temperature dataset] was created that used maximum likelihood estimation (MLE) to combine the land surface ...1 week ago
Related Posts
- Release: Charter schools to remove the rights of teachers
 A late change to charter school legislation will cheat educators out of fair pay and negotiating power proving charter schools are just a vehicle to make profit out of our education system. ...23 hours ago
A late change to charter school legislation will cheat educators out of fair pay and negotiating power proving charter schools are just a vehicle to make profit out of our education system. ...23 hours ago - Te iwi Māori will not stand for another Foreshore and Seabed
 In 2004 te iwi Māori rallied against the Crown’s attempt to confiscate our coastlines and moana with the Foreshore and Seabed Act. This led to the largest hīkoi of a generation and the birth of Te Pāti Māori. 20 years later, history is repeating itself. Today the government has announced ...2 days ago
In 2004 te iwi Māori rallied against the Crown’s attempt to confiscate our coastlines and moana with the Foreshore and Seabed Act. This led to the largest hīkoi of a generation and the birth of Te Pāti Māori. 20 years later, history is repeating itself. Today the government has announced ...2 days ago - Te Pāti Māori Acknowledge the Need for Fundamental Change in State Care
 It has been five and a half years since the Royal Commission of Inquiry into Abuse in Care was established to investigate the abuse of children, young people, and vulnerable adults within state and faith-based institutions. Yesterday, the final report - Whanaketia through pain and trauma, from darkness to light ...2 days ago
It has been five and a half years since the Royal Commission of Inquiry into Abuse in Care was established to investigate the abuse of children, young people, and vulnerable adults within state and faith-based institutions. Yesterday, the final report - Whanaketia through pain and trauma, from darkness to light ...2 days ago - National disgrace for children in poverty
2 days ago
- Release: National disgrace for children in poverty
2 days ago
- Government quietly waters down child poverty targets
 The Government’s move to dilute child poverty targets is a reminder that it is actively choosing to preserve hardship for thousands of households. ...2 days ago
The Government’s move to dilute child poverty targets is a reminder that it is actively choosing to preserve hardship for thousands of households. ...2 days ago - Release: National jumps on Labour’s trains
 National is so short on ideas it is now announcing Labour’s rail announcement from a year ago, Labour transport spokesperson Tangi Utikere said. ...2 days ago
National is so short on ideas it is now announcing Labour’s rail announcement from a year ago, Labour transport spokesperson Tangi Utikere said. ...2 days ago - Release: Opposition parties unite to protect ECE
 Labour, the Green Party and Te Pāti Māori are uniting to stop the Government’s dangerous changes to the Early Childhood Education sector. ...2 days ago
Labour, the Green Party and Te Pāti Māori are uniting to stop the Government’s dangerous changes to the Early Childhood Education sector. ...2 days ago - Release: Another step forward for survivors of abuse in care
 Labour welcomes the Royal Commission of Inquiry into Abuse in Care’s final report and the government committing to a formal apology in November. ...3 days ago
Labour welcomes the Royal Commission of Inquiry into Abuse in Care’s final report and the government committing to a formal apology in November. ...3 days ago - Govt must listen to experiences of abuse survivors
 The Government must do all it can to bring abuse in care to an end following the release of the independent inquiry. ...3 days ago
The Government must do all it can to bring abuse in care to an end following the release of the independent inquiry. ...3 days ago - Release: Health New Zealand exposes Minister spinning in freefall
 Health New Zealand contradicted the Government’s spin that back-office bureaucracy is the cause of overspend in the public health system. ...4 days ago
Health New Zealand contradicted the Government’s spin that back-office bureaucracy is the cause of overspend in the public health system. ...4 days ago - Govt must act on Israel’s illegal occupation of Palestine
 The Green Party is calling on the Government to take action off the back of the International Court of Justice ruling on Israel’s illegal occupation of Palestine. ...4 days ago
The Green Party is calling on the Government to take action off the back of the International Court of Justice ruling on Israel’s illegal occupation of Palestine. ...4 days ago - NZ Government Must Enforce ICJ Ruling
 On Friday the International Court of Justice reaffirmed what Palestinian’s have been telling us for decades: that the occupation and colonisation of Palestinian lands by Israel is illegal and must end immediately. They also called for reparations for Palestinian’s who have lived under Israeli occupation since it began in 1967. ...5 days ago
On Friday the International Court of Justice reaffirmed what Palestinian’s have been telling us for decades: that the occupation and colonisation of Palestinian lands by Israel is illegal and must end immediately. They also called for reparations for Palestinian’s who have lived under Israeli occupation since it began in 1967. ...5 days ago - Release: Listen PM, boot camps don’t work
 Refusing to listen to evidence, experts or experience the Government is stubbornly marching ahead with its boot camps. ...7 days ago
Refusing to listen to evidence, experts or experience the Government is stubbornly marching ahead with its boot camps. ...7 days ago - Release: Govt must act on ICJ ruling on illegal Israeli occupation
 Labour calls on the Government to act after the International Court of Justice (ICJ) ruled that Israel’s occupation of Palestinian Territories is illegal. ...7 days ago
Labour calls on the Government to act after the International Court of Justice (ICJ) ruled that Israel’s occupation of Palestinian Territories is illegal. ...7 days ago - Release: Rents up under National, promises fall flat
 National Party policies which promised to put “downward pressure” on rents are having the opposite effect. ...1 week ago
National Party policies which promised to put “downward pressure” on rents are having the opposite effect. ...1 week ago - MSD figures show Govt determined to punish beneficiaries
 The 53.7 percent rise in benefit sanctions over the last year is more proof of this Government’s disdain for our communities most in need of support. ...1 week ago
The 53.7 percent rise in benefit sanctions over the last year is more proof of this Government’s disdain for our communities most in need of support. ...1 week ago - We need real solutions, not more failed boot camps – Willow-Jean Prime
 Aotearoa could be a country where every child grows up feeling safe, loved and with a sense of belonging in their whānau and community. But for some of our children, this is far from reality. Instead, they are trapped in a maze of intergenerational harm that they can’t escape on ...1 week ago
Aotearoa could be a country where every child grows up feeling safe, loved and with a sense of belonging in their whānau and community. But for some of our children, this is far from reality. Instead, they are trapped in a maze of intergenerational harm that they can’t escape on ...1 week ago - David Seymour is Unfit to Serve as Minister
 Te Pāti Māori are calling for David Seymour to resign as Associate Health Minister in response to his call for Pharmac to ignore the Treaty of Waitangi. “This announcement is just another example of the government’s anti-Tiriti, anti-Māori agenda.” Said Co-leader and spokesperson for health, Debbie Ngarewa-Packer. “Seymour thinks it ...1 week ago
Te Pāti Māori are calling for David Seymour to resign as Associate Health Minister in response to his call for Pharmac to ignore the Treaty of Waitangi. “This announcement is just another example of the government’s anti-Tiriti, anti-Māori agenda.” Said Co-leader and spokesperson for health, Debbie Ngarewa-Packer. “Seymour thinks it ...1 week ago - Renters suffer as soaring rents feed rising inflation
 The soaring price of renting is driving the rise of inflation in this country - with latest figures from Stats NZ showing rents are up 4.8 per cent on average while annual inflation is at 3.3 per cent. ...1 week ago
The soaring price of renting is driving the rise of inflation in this country - with latest figures from Stats NZ showing rents are up 4.8 per cent on average while annual inflation is at 3.3 per cent. ...1 week ago - National’s climate strategy undoes good progress
 National’s Emissions Reduction Plan will take New Zealand further from the economy we need to ensure the next generation has a stable climate and secure livelihoods. ...1 week ago
National’s Emissions Reduction Plan will take New Zealand further from the economy we need to ensure the next generation has a stable climate and secure livelihoods. ...1 week ago - Green Party releases executive summary of independent investigation
 Following consultation with named parties and thorough consideration of privacy interests, the Green Party is in a position to release the Executive Summary of the final report from the independent investigation into Darleen Tana. ...1 week ago
Following consultation with named parties and thorough consideration of privacy interests, the Green Party is in a position to release the Executive Summary of the final report from the independent investigation into Darleen Tana. ...1 week ago - Government back off track on climate action
 Today’s Draft Emissions Reduction Plan shows the Government couldn’t care less about a liveable climate for all. ...1 week ago
Today’s Draft Emissions Reduction Plan shows the Government couldn’t care less about a liveable climate for all. ...1 week ago - PM needs to step in over Shane Jones’ undeclared meeting
 Prime Minister Christopher Luxon should be asking serious questions of his Minister for Resources Shane Jones now it’s been revealed he misled the public about a dinner with mining companies that he didn’t declare and said wasn’t pre-arranged. ...2 weeks ago
Prime Minister Christopher Luxon should be asking serious questions of his Minister for Resources Shane Jones now it’s been revealed he misled the public about a dinner with mining companies that he didn’t declare and said wasn’t pre-arranged. ...2 weeks ago - Te Pāti Māori Opposes Three Strikes Amendment Bill
 Te Pāti Māori have submitted to the Justice Select Committee against the Sentencing (Reinstating Three Strikes) Amendment Bill. The bill will further entrench racism in our justice system and fails to focus on rehabilitation. “Reinstating Three Strikes will empower a systematically racist system and exacerbate the overrepresentation of Māori in ...2 weeks ago
Te Pāti Māori have submitted to the Justice Select Committee against the Sentencing (Reinstating Three Strikes) Amendment Bill. The bill will further entrench racism in our justice system and fails to focus on rehabilitation. “Reinstating Three Strikes will empower a systematically racist system and exacerbate the overrepresentation of Māori in ...2 weeks ago - Govt Determined to Make Aotearoa a Country of Disposable Renters
 The Transport and Infrastructure Committee is set to make a determination on the Residential Tenancies Amendment (RTA) Bill in the coming weeks. “This legislation will give landlords the power to kick our whānau out onto the street for no reason” said Housing spokesperson, Mariameno Kapa-Kingi. “Their solution to the housing ...2 weeks ago
The Transport and Infrastructure Committee is set to make a determination on the Residential Tenancies Amendment (RTA) Bill in the coming weeks. “This legislation will give landlords the power to kick our whānau out onto the street for no reason” said Housing spokesperson, Mariameno Kapa-Kingi. “Their solution to the housing ...2 weeks ago - Statement on retail crime Ministerial Advisory Group
 “National’s campaign was about tackling crime and the best they can do is a two-year long Ministerial Advisory Group,” Labour justice spokesperson Duncan Webb said. ...2 weeks ago
“National’s campaign was about tackling crime and the best they can do is a two-year long Ministerial Advisory Group,” Labour justice spokesperson Duncan Webb said. ...2 weeks ago - Statement from Labour education spokesperson Jan Tinetti
 “There are more examples of charter schools failing their students than there are success stories. The coalition Government is driving to dismantle our public school system and instead promote a privatised, competitive structure that puts profits before kids,” Jan Tinetti said. ...2 weeks ago
“There are more examples of charter schools failing their students than there are success stories. The coalition Government is driving to dismantle our public school system and instead promote a privatised, competitive structure that puts profits before kids,” Jan Tinetti said. ...2 weeks ago - Govt Continues to Destructively Withhold Information
 “This government is choosing to deliberately mislead and withhold information, keeping our people in the dark about this government’s agenda and the future of our mokopuna,” said co-leader and spokesperson for Health, Debbie Ngarewa-Packer. The call comes after the demand from the Chief Ombudsman that Associate Minister of Health, Casey ...2 weeks ago
“This government is choosing to deliberately mislead and withhold information, keeping our people in the dark about this government’s agenda and the future of our mokopuna,” said co-leader and spokesperson for Health, Debbie Ngarewa-Packer. The call comes after the demand from the Chief Ombudsman that Associate Minister of Health, Casey ...2 weeks ago - Statement from Labour climate change spokesperson Megan Woods
 “Today’s climate announcement by Simon Watts makes clear the National Government is simply paying lip service to meeting its climate change targets,” Megan Woods said. ...2 weeks ago
“Today’s climate announcement by Simon Watts makes clear the National Government is simply paying lip service to meeting its climate change targets,” Megan Woods said. ...2 weeks ago - Eight ways National is making life harder for workers
 National is choosing to make life harder for workers by taking away the rights our communities have fought hard for. Here's how they’re taking workers backwards. ...3 weeks ago
National is choosing to make life harder for workers by taking away the rights our communities have fought hard for. Here's how they’re taking workers backwards. ...3 weeks ago - Waitlists up and workforce down under National
 Health New Zealand’s recent quarterly performance report shows the public health system is going backwards under the National government. ...3 weeks ago
Health New Zealand’s recent quarterly performance report shows the public health system is going backwards under the National government. ...3 weeks ago
Related Posts
- Joint statement from the Prime Ministers of Canada, Australia and New Zealand
 Australia, Canada and New Zealand today issued the following statement on the need for an urgent ceasefire in Gaza and the risk of expanded conflict between Hizballah and Israel. The situation in Gaza is catastrophic. The human suffering is unacceptable. It cannot continue. We remain unequivocal in our condemnation of ...BeehiveBy beehive.govt.nz17 hours ago
Australia, Canada and New Zealand today issued the following statement on the need for an urgent ceasefire in Gaza and the risk of expanded conflict between Hizballah and Israel. The situation in Gaza is catastrophic. The human suffering is unacceptable. It cannot continue. We remain unequivocal in our condemnation of ...BeehiveBy beehive.govt.nz17 hours ago - AG reminds institutions of legal obligations
 Attorney-General Judith Collins today reminded all State and faith-based institutions of their legal obligation to preserve records relevant to the safety and wellbeing of those in its care. “The Abuse in Care Inquiry’s report has found cases where records of the most vulnerable people in State and faith‑based institutions were ...BeehiveBy beehive.govt.nz19 hours ago
Attorney-General Judith Collins today reminded all State and faith-based institutions of their legal obligation to preserve records relevant to the safety and wellbeing of those in its care. “The Abuse in Care Inquiry’s report has found cases where records of the most vulnerable people in State and faith‑based institutions were ...BeehiveBy beehive.govt.nz19 hours ago - More young people learning about digital safety
 Minister of Internal Affairs Brooke van Velden says the Government’s online safety website for children and young people has reached one million page views. “It is great to see so many young people and their families accessing the site Keep It Real Online to learn how to stay safe online, and manage ...BeehiveBy beehive.govt.nz20 hours ago
Minister of Internal Affairs Brooke van Velden says the Government’s online safety website for children and young people has reached one million page views. “It is great to see so many young people and their families accessing the site Keep It Real Online to learn how to stay safe online, and manage ...BeehiveBy beehive.govt.nz20 hours ago - Speech to the Conference for General Practice 2024
 Tēnā tātou katoa, Ngā mihi te rangi, ngā mihi te whenua, ngā mihi ki a koutou, kia ora mai koutou. Thank you for the opportunity to be here and the invitation to speak at this 50th anniversary conference. I acknowledge all those who have gone before us and paved the ...BeehiveBy beehive.govt.nz22 hours ago
Tēnā tātou katoa, Ngā mihi te rangi, ngā mihi te whenua, ngā mihi ki a koutou, kia ora mai koutou. Thank you for the opportunity to be here and the invitation to speak at this 50th anniversary conference. I acknowledge all those who have gone before us and paved the ...BeehiveBy beehive.govt.nz22 hours ago - Employers and payroll providers ready for tax changes
 New Zealand’s payroll providers have successfully prepared to ensure 3.5 million individuals will, from Wednesday next week, be able to keep more of what they earn each pay, says Finance Minister Nicola Willis and Revenue Minister Simon Watts. “The Government's tax policy changes are legally effective from Wednesday. Delivering this tax ...BeehiveBy beehive.govt.nz24 hours ago
New Zealand’s payroll providers have successfully prepared to ensure 3.5 million individuals will, from Wednesday next week, be able to keep more of what they earn each pay, says Finance Minister Nicola Willis and Revenue Minister Simon Watts. “The Government's tax policy changes are legally effective from Wednesday. Delivering this tax ...BeehiveBy beehive.govt.nz24 hours ago - Experimental vineyard futureproofs wine industry
 An experimental vineyard which will help futureproof the wine sector has been opened in Blenheim by Associate Regional Development Minister Mark Patterson. The covered vineyard, based at the New Zealand Wine Centre – Te Pokapū Wāina o Aotearoa, enables controlled environmental conditions. “The research that will be produced at the Experimental ...BeehiveBy beehive.govt.nz1 day ago
An experimental vineyard which will help futureproof the wine sector has been opened in Blenheim by Associate Regional Development Minister Mark Patterson. The covered vineyard, based at the New Zealand Wine Centre – Te Pokapū Wāina o Aotearoa, enables controlled environmental conditions. “The research that will be produced at the Experimental ...BeehiveBy beehive.govt.nz1 day ago - Funding confirmed for regions affected by North Island Weather Events
 The Coalition Government has confirmed the indicative regional breakdown of North Island Weather Event (NIWE) funding for state highway recovery projects funded through Budget 2024, Transport Minister Simeon Brown says. “Regions in the North Island suffered extensive and devastating damage from Cyclone Gabrielle and the 2023 Auckland Anniversary Floods, and ...BeehiveBy beehive.govt.nz1 day ago
The Coalition Government has confirmed the indicative regional breakdown of North Island Weather Event (NIWE) funding for state highway recovery projects funded through Budget 2024, Transport Minister Simeon Brown says. “Regions in the North Island suffered extensive and devastating damage from Cyclone Gabrielle and the 2023 Auckland Anniversary Floods, and ...BeehiveBy beehive.govt.nz1 day ago - Indonesian Foreign Minister to visit
 Indonesia’s Foreign Minister, Retno Marsudi, will visit New Zealand next week, Foreign Minister Winston Peters has announced. “Indonesia is important to New Zealand’s security and economic interests and is our closest South East Asian neighbour,” says Mr Peters, who is currently in Laos to engage with South East Asian partners. ...BeehiveBy beehive.govt.nz1 day ago
Indonesia’s Foreign Minister, Retno Marsudi, will visit New Zealand next week, Foreign Minister Winston Peters has announced. “Indonesia is important to New Zealand’s security and economic interests and is our closest South East Asian neighbour,” says Mr Peters, who is currently in Laos to engage with South East Asian partners. ...BeehiveBy beehive.govt.nz1 day ago - Strengthening partnership with Ngāti Maniapoto
 He aha te kai a te rangatira? He kōrero, he kōrero, he kōrero. The government has reaffirmed its commitment to supporting the aspirations of Ngāti Maniapoto, Minister for Māori Development Tama Potaka says. “My thanks to Te Nehenehenui Trust – Ngāti Maniapoto for bringing their important kōrero to a ministerial ...BeehiveBy beehive.govt.nz2 days ago
He aha te kai a te rangatira? He kōrero, he kōrero, he kōrero. The government has reaffirmed its commitment to supporting the aspirations of Ngāti Maniapoto, Minister for Māori Development Tama Potaka says. “My thanks to Te Nehenehenui Trust – Ngāti Maniapoto for bringing their important kōrero to a ministerial ...BeehiveBy beehive.govt.nz2 days ago - Transport Minister thanks outgoing CAA Chair
 Transport Minister Simeon Brown has thanked outgoing Chair of the Civil Aviation Authority, Janice Fredric, for her service to the board.“I have received Ms Fredric’s resignation from the role of Chair of the Civil Aviation Authority,” Mr Brown says.“On behalf of the Government, I want to thank Ms Fredric for ...BeehiveBy beehive.govt.nz2 days ago
Transport Minister Simeon Brown has thanked outgoing Chair of the Civil Aviation Authority, Janice Fredric, for her service to the board.“I have received Ms Fredric’s resignation from the role of Chair of the Civil Aviation Authority,” Mr Brown says.“On behalf of the Government, I want to thank Ms Fredric for ...BeehiveBy beehive.govt.nz2 days ago - Test for Customary Marine Title being restored
 The Government is proposing legislation to overturn a Court of Appeal decision and amend the Marine and Coastal Area Act in order to restore Parliament’s test for Customary Marine Title, Treaty Negotiations Minister Paul Goldsmith says. “Section 58 required an applicant group to prove they have exclusively used and occupied ...BeehiveBy beehive.govt.nz2 days ago
The Government is proposing legislation to overturn a Court of Appeal decision and amend the Marine and Coastal Area Act in order to restore Parliament’s test for Customary Marine Title, Treaty Negotiations Minister Paul Goldsmith says. “Section 58 required an applicant group to prove they have exclusively used and occupied ...BeehiveBy beehive.govt.nz2 days ago - Opposition united in bad faith over ECE sector review
 Regulation Minister David Seymour says that opposition parties have united in bad faith, opposing what they claim are ‘dangerous changes’ to the Early Childhood Education sector, despite no changes even being proposed yet. “Issues with affordability and availability of early childhood education, and the complexity of its regulation, has led ...BeehiveBy beehive.govt.nz2 days ago
Regulation Minister David Seymour says that opposition parties have united in bad faith, opposing what they claim are ‘dangerous changes’ to the Early Childhood Education sector, despite no changes even being proposed yet. “Issues with affordability and availability of early childhood education, and the complexity of its regulation, has led ...BeehiveBy beehive.govt.nz2 days ago - Kiwis having their say on first regulatory review
 After receiving more than 740 submissions in the first 20 days, Regulation Minister David Seymour is asking the Ministry for Regulation to extend engagement on the early childhood education regulation review by an extra two weeks. “The level of interest has been very high, and from the conversations I’ve been ...BeehiveBy beehive.govt.nz2 days ago
After receiving more than 740 submissions in the first 20 days, Regulation Minister David Seymour is asking the Ministry for Regulation to extend engagement on the early childhood education regulation review by an extra two weeks. “The level of interest has been very high, and from the conversations I’ve been ...BeehiveBy beehive.govt.nz2 days ago - Government upgrading Lower North Island commuter rail
 The Coalition Government is investing $802.9 million into the Wairarapa and Manawatū rail lines as part of a funding agreement with the NZ Transport Agency (NZTA), KiwiRail, and the Greater Wellington and Horizons Regional Councils to deliver more reliable services for commuters in the lower North Island, Transport Minister Simeon ...BeehiveBy beehive.govt.nz2 days ago
The Coalition Government is investing $802.9 million into the Wairarapa and Manawatū rail lines as part of a funding agreement with the NZ Transport Agency (NZTA), KiwiRail, and the Greater Wellington and Horizons Regional Councils to deliver more reliable services for commuters in the lower North Island, Transport Minister Simeon ...BeehiveBy beehive.govt.nz2 days ago - Government moves to ensure flood protection for Wairoa
 Local Government Minister Simeon Brown has announced his intention to appoint a Crown Manager to both Hawke’s Bay Regional and Wairoa District Councils to speed up the delivery of flood protection work in Wairoa."Recent severe weather events in Wairoa this year, combined with damage from Cyclone Gabrielle in 2023 have ...BeehiveBy beehive.govt.nz3 days ago
Local Government Minister Simeon Brown has announced his intention to appoint a Crown Manager to both Hawke’s Bay Regional and Wairoa District Councils to speed up the delivery of flood protection work in Wairoa."Recent severe weather events in Wairoa this year, combined with damage from Cyclone Gabrielle in 2023 have ...BeehiveBy beehive.govt.nz3 days ago - PM speech to Parliament – Royal Commission of Inquiry’s Report into Abuse in Care
 Mr Speaker, this is a day that many New Zealanders who were abused in State care never thought would come. It’s the day that this Parliament accepts, with deep sorrow and regret, the Report of the Royal Commission of Inquiry into Abuse in Care. At the heart of this report are the ...BeehiveBy beehive.govt.nz3 days ago
Mr Speaker, this is a day that many New Zealanders who were abused in State care never thought would come. It’s the day that this Parliament accepts, with deep sorrow and regret, the Report of the Royal Commission of Inquiry into Abuse in Care. At the heart of this report are the ...BeehiveBy beehive.govt.nz3 days ago - Government acknowledges torture at Lake Alice
 For the first time, the Government is formally acknowledging some children and young people at Lake Alice Psychiatric Hospital experienced torture. The final report of the Royal Commission of Inquiry into Abuse in State and Faith-based Care “Whanaketia – through pain and trauma, from darkness to light,” was tabled in Parliament ...BeehiveBy beehive.govt.nz3 days ago
For the first time, the Government is formally acknowledging some children and young people at Lake Alice Psychiatric Hospital experienced torture. The final report of the Royal Commission of Inquiry into Abuse in State and Faith-based Care “Whanaketia – through pain and trauma, from darkness to light,” was tabled in Parliament ...BeehiveBy beehive.govt.nz3 days ago - Government acknowledges courageous abuse survivors
 The Government has acknowledged the nearly 2,400 courageous survivors who shared their experiences during the Royal Commission of Inquiry into Historical Abuse in State and Faith-Based Care. The final report from the largest and most complex public inquiry ever held in New Zealand, the Royal Commission Inquiry “Whanaketia – through ...BeehiveBy beehive.govt.nz3 days ago
The Government has acknowledged the nearly 2,400 courageous survivors who shared their experiences during the Royal Commission of Inquiry into Historical Abuse in State and Faith-Based Care. The final report from the largest and most complex public inquiry ever held in New Zealand, the Royal Commission Inquiry “Whanaketia – through ...BeehiveBy beehive.govt.nz3 days ago - Half a million people use tax calculator
 With a week to go before hard-working New Zealanders see personal income tax relief for the first time in fourteen years, 513,000 people have used the Budget tax calculator to see how much they will benefit, says Finance Minister Nicola Willis. “Tax relief is long overdue. From next Wednesday, personal income ...BeehiveBy beehive.govt.nz3 days ago
With a week to go before hard-working New Zealanders see personal income tax relief for the first time in fourteen years, 513,000 people have used the Budget tax calculator to see how much they will benefit, says Finance Minister Nicola Willis. “Tax relief is long overdue. From next Wednesday, personal income ...BeehiveBy beehive.govt.nz3 days ago - Paid Parental Leave improvements pass first reading
 Workplace Relations and Safety Minister Brooke van Velden says a bill that has passed its first reading will improve parental leave settings and give non-biological parents more flexibility as primary carer for their child. The Regulatory Systems Amendment Bill (No3), passed its first reading this morning. “It includes a change ...BeehiveBy beehive.govt.nz3 days ago
Workplace Relations and Safety Minister Brooke van Velden says a bill that has passed its first reading will improve parental leave settings and give non-biological parents more flexibility as primary carer for their child. The Regulatory Systems Amendment Bill (No3), passed its first reading this morning. “It includes a change ...BeehiveBy beehive.govt.nz3 days ago - Rebuilding the economy through better regulation
 Two Bills designed to improve regulation and make it easier to do business have passed their first reading in Parliament, says Economic Development Minister Melissa Lee. The Regulatory Systems (Economic Development) Amendment Bill and Regulatory Systems (Immigration and Workforce) Amendment Bill make key changes to legislation administered by the Ministry ...BeehiveBy beehive.govt.nz3 days ago
Two Bills designed to improve regulation and make it easier to do business have passed their first reading in Parliament, says Economic Development Minister Melissa Lee. The Regulatory Systems (Economic Development) Amendment Bill and Regulatory Systems (Immigration and Workforce) Amendment Bill make key changes to legislation administered by the Ministry ...BeehiveBy beehive.govt.nz3 days ago - ‘Open banking’ and ‘open electricity’ on the way
 New legislation paves the way for greater competition in sectors such as banking and electricity, Commerce and Consumer Affairs Minister Andrew Bayly says. “Competitive markets boost productivity, create employment opportunities and lift living standards. To support competition, we need good quality regulation but, unfortunately, a recent OECD report ranked New ...BeehiveBy beehive.govt.nz3 days ago
New legislation paves the way for greater competition in sectors such as banking and electricity, Commerce and Consumer Affairs Minister Andrew Bayly says. “Competitive markets boost productivity, create employment opportunities and lift living standards. To support competition, we need good quality regulation but, unfortunately, a recent OECD report ranked New ...BeehiveBy beehive.govt.nz3 days ago - Charity lotteries to be permitted to operate online
 Minister of Internal Affairs Brooke van Velden says lotteries for charitable purposes, such as those run by the Heart Foundation, Coastguard NZ, and local hospices, will soon be allowed to operate online permanently. “Under current laws, these fundraising lotteries are only allowed to operate online until October 2024, after which ...BeehiveBy beehive.govt.nz4 days ago
Minister of Internal Affairs Brooke van Velden says lotteries for charitable purposes, such as those run by the Heart Foundation, Coastguard NZ, and local hospices, will soon be allowed to operate online permanently. “Under current laws, these fundraising lotteries are only allowed to operate online until October 2024, after which ...BeehiveBy beehive.govt.nz4 days ago - Accelerating Northland Expressway
 The Coalition Government is accelerating work on the new four-lane expressway between Auckland and Whangārei as part of its Roads of National Significance programme, with an accelerated delivery model to deliver this project faster and more efficiently, Transport Minister Simeon Brown says. “For too long, the lack of resilient transport connections ...BeehiveBy beehive.govt.nz4 days ago
The Coalition Government is accelerating work on the new four-lane expressway between Auckland and Whangārei as part of its Roads of National Significance programme, with an accelerated delivery model to deliver this project faster and more efficiently, Transport Minister Simeon Brown says. “For too long, the lack of resilient transport connections ...BeehiveBy beehive.govt.nz4 days ago - Sir Don to travel to Viet Nam as special envoy
 Sir Don McKinnon will travel to Viet Nam this week as a Special Envoy of the Government, Foreign Minister Winston Peters has announced. “It is important that the Government give due recognition to the significant contributions that General Secretary Nguyen Phu Trong made to New Zealand-Viet Nam relations,” Mr ...BeehiveBy beehive.govt.nz4 days ago
Sir Don McKinnon will travel to Viet Nam this week as a Special Envoy of the Government, Foreign Minister Winston Peters has announced. “It is important that the Government give due recognition to the significant contributions that General Secretary Nguyen Phu Trong made to New Zealand-Viet Nam relations,” Mr ...BeehiveBy beehive.govt.nz4 days ago - Grant Illingworth KC appointed as transitional Commissioner to Royal Commission
 Minister of Internal Affairs Brooke van Velden says newly appointed Commissioner, Grant Illingworth KC, will help deliver the report for the first phase of the Royal Commission of Inquiry into COVID-19 Lessons, due on 28 November 2024. “I am pleased to announce that Mr Illingworth will commence his appointment as ...BeehiveBy beehive.govt.nz4 days ago
Minister of Internal Affairs Brooke van Velden says newly appointed Commissioner, Grant Illingworth KC, will help deliver the report for the first phase of the Royal Commission of Inquiry into COVID-19 Lessons, due on 28 November 2024. “I am pleased to announce that Mr Illingworth will commence his appointment as ...BeehiveBy beehive.govt.nz4 days ago - NZ to advance relationships with ASEAN partners
 Foreign Minister Winston Peters travels to Laos this week to participate in a series of Association of Southeast Asian Nations (ASEAN)-led Ministerial meetings in Vientiane. “ASEAN plays an important role in supporting a peaceful, stable and prosperous Indo-Pacific,” Mr Peters says. “This will be our third visit to ...BeehiveBy beehive.govt.nz4 days ago
Foreign Minister Winston Peters travels to Laos this week to participate in a series of Association of Southeast Asian Nations (ASEAN)-led Ministerial meetings in Vientiane. “ASEAN plays an important role in supporting a peaceful, stable and prosperous Indo-Pacific,” Mr Peters says. “This will be our third visit to ...BeehiveBy beehive.govt.nz4 days ago - Backing mental health services on the West Coast
 Construction of a new mental health facility at Te Nikau Grey Hospital in Greymouth is today one step closer, Mental Health Minister Matt Doocey says. “This $27 million facility shows this Government is delivering on its promise to boost mental health care and improve front line services,” Mr Doocey says. ...BeehiveBy beehive.govt.nz4 days ago
Construction of a new mental health facility at Te Nikau Grey Hospital in Greymouth is today one step closer, Mental Health Minister Matt Doocey says. “This $27 million facility shows this Government is delivering on its promise to boost mental health care and improve front line services,” Mr Doocey says. ...BeehiveBy beehive.govt.nz4 days ago - NZ support for sustainable Pacific fisheries
 New Zealand is committing nearly $50 million to a package supporting sustainable Pacific fisheries development over the next four years, Foreign Minister Winston Peters and Oceans and Fisheries Minister Shane Jones announced today. “This support consisting of a range of initiatives demonstrates New Zealand’s commitment to assisting our Pacific partners ...BeehiveBy beehive.govt.nz4 days ago
New Zealand is committing nearly $50 million to a package supporting sustainable Pacific fisheries development over the next four years, Foreign Minister Winston Peters and Oceans and Fisheries Minister Shane Jones announced today. “This support consisting of a range of initiatives demonstrates New Zealand’s commitment to assisting our Pacific partners ...BeehiveBy beehive.govt.nz4 days ago - Students’ needs at centre of new charter school adjustments
 Associate Education Minister David Seymour says proposed changes to the Education and Training Amendment Bill will ensure charter schools have more flexibility to negotiate employment agreements and are equipped with the right teaching resources. “Cabinet has agreed to progress an amendment which means unions will not be able to initiate ...BeehiveBy beehive.govt.nz4 days ago
Associate Education Minister David Seymour says proposed changes to the Education and Training Amendment Bill will ensure charter schools have more flexibility to negotiate employment agreements and are equipped with the right teaching resources. “Cabinet has agreed to progress an amendment which means unions will not be able to initiate ...BeehiveBy beehive.govt.nz4 days ago - Commissioner replaces Health NZ Board
 In response to serious concerns around oversight, overspend and a significant deterioration in financial outlook, the Board of Health New Zealand will be replaced with a Commissioner, Health Minister Dr Shane Reti announced today. “The previous government’s botched health reforms have created significant financial challenges at Health NZ that, without ...BeehiveBy beehive.govt.nz5 days ago
In response to serious concerns around oversight, overspend and a significant deterioration in financial outlook, the Board of Health New Zealand will be replaced with a Commissioner, Health Minister Dr Shane Reti announced today. “The previous government’s botched health reforms have created significant financial challenges at Health NZ that, without ...BeehiveBy beehive.govt.nz5 days ago - Minister to speak at Australian Space Forum
 Minister for Space and Science, Innovation and Technology Judith Collins will travel to Adelaide tomorrow for space and science engagements, including speaking at the Australian Space Forum. While there she will also have meetings and visits with a focus on space, biotechnology and innovation. “New Zealand has a thriving space ...BeehiveBy beehive.govt.nz5 days ago
Minister for Space and Science, Innovation and Technology Judith Collins will travel to Adelaide tomorrow for space and science engagements, including speaking at the Australian Space Forum. While there she will also have meetings and visits with a focus on space, biotechnology and innovation. “New Zealand has a thriving space ...BeehiveBy beehive.govt.nz5 days ago - Climate Change Minister to attend climate action meeting in China
 Climate Change Minister Simon Watts will travel to China on Saturday to attend the Ministerial on Climate Action meeting held in Wuhan. “Attending the Ministerial on Climate Action is an opportunity to advocate for New Zealand climate priorities and engage with our key partners on climate action,” Mr Watts says. ...BeehiveBy beehive.govt.nz5 days ago
Climate Change Minister Simon Watts will travel to China on Saturday to attend the Ministerial on Climate Action meeting held in Wuhan. “Attending the Ministerial on Climate Action is an opportunity to advocate for New Zealand climate priorities and engage with our key partners on climate action,” Mr Watts says. ...BeehiveBy beehive.govt.nz5 days ago - Oceans and Fisheries Minister to Solomons
 Oceans and Fisheries Minister Shane Jones is travelling to the Solomon Islands tomorrow for meetings with his counterparts from around the Pacific supporting collective management of the region’s fisheries. The 23rd Pacific Islands Forum Fisheries Committee and the 5th Regional Fisheries Ministers’ Meeting in Honiara from 23 to 26 July ...BeehiveBy beehive.govt.nz7 days ago
Oceans and Fisheries Minister Shane Jones is travelling to the Solomon Islands tomorrow for meetings with his counterparts from around the Pacific supporting collective management of the region’s fisheries. The 23rd Pacific Islands Forum Fisheries Committee and the 5th Regional Fisheries Ministers’ Meeting in Honiara from 23 to 26 July ...BeehiveBy beehive.govt.nz7 days ago - Government launches Military Style Academy Pilot
 The Government today launched the Military Style Academy Pilot at Te Au rere a te Tonga Youth Justice residence in Palmerston North, an important part of the Government’s plan to crackdown on youth crime and getting youth offenders back on track, Minister for Children, Karen Chhour said today. “On the ...BeehiveBy beehive.govt.nz7 days ago
The Government today launched the Military Style Academy Pilot at Te Au rere a te Tonga Youth Justice residence in Palmerston North, an important part of the Government’s plan to crackdown on youth crime and getting youth offenders back on track, Minister for Children, Karen Chhour said today. “On the ...BeehiveBy beehive.govt.nz7 days ago - Nine priority bridge replacements to get underway
 The Government has welcomed news the NZ Transport Agency (NZTA) has begun work to replace nine priority bridges across the country to ensure our state highway network remains resilient, reliable, and efficient for road users, Transport Minister Simeon Brown says.“Increasing productivity and economic growth is a key priority for the ...BeehiveBy beehive.govt.nz1 week ago
The Government has welcomed news the NZ Transport Agency (NZTA) has begun work to replace nine priority bridges across the country to ensure our state highway network remains resilient, reliable, and efficient for road users, Transport Minister Simeon Brown says.“Increasing productivity and economic growth is a key priority for the ...BeehiveBy beehive.govt.nz1 week ago - Update on global IT outage
 Acting Prime Minister David Seymour has been in contact throughout the evening with senior officials who have coordinated a whole of government response to the global IT outage and can provide an update. The Department of the Prime Minister and Cabinet has designated the National Emergency Management Agency as the ...BeehiveBy beehive.govt.nz1 week ago
Acting Prime Minister David Seymour has been in contact throughout the evening with senior officials who have coordinated a whole of government response to the global IT outage and can provide an update. The Department of the Prime Minister and Cabinet has designated the National Emergency Management Agency as the ...BeehiveBy beehive.govt.nz1 week ago - New Zealand, Japan renew Pacific partnership
 New Zealand and Japan will continue to step up their shared engagement with the Pacific, Foreign Minister Winston Peters says. “New Zealand and Japan have a strong, shared interest in a free, open and stable Pacific Islands region,” Mr Peters says. “We are pleased to be finding more ways ...BeehiveBy beehive.govt.nz1 week ago
New Zealand and Japan will continue to step up their shared engagement with the Pacific, Foreign Minister Winston Peters says. “New Zealand and Japan have a strong, shared interest in a free, open and stable Pacific Islands region,” Mr Peters says. “We are pleased to be finding more ways ...BeehiveBy beehive.govt.nz1 week ago - New infrastructure energises BOP forestry towns
 New developments in the heart of North Island forestry country will reinvigorate their communities and boost economic development, Regional Development Minister Shane Jones says. Mr Jones visited Kaingaroa and Kawerau in Bay of Plenty today to open a landmark community centre in the former and a new connecting road in ...BeehiveBy beehive.govt.nz1 week ago
New developments in the heart of North Island forestry country will reinvigorate their communities and boost economic development, Regional Development Minister Shane Jones says. Mr Jones visited Kaingaroa and Kawerau in Bay of Plenty today to open a landmark community centre in the former and a new connecting road in ...BeehiveBy beehive.govt.nz1 week ago - 'Pacific Futures'
 President Adeang, fellow Ministers, honourable Diet Member Horii, Ambassadors, distinguished guests. Minasama, konnichiwa, and good afternoon, everyone. Distinguished guests, it’s a pleasure to be here with you today to talk about New Zealand’s foreign policy reset, the reasons for it, the values that underpin it, and how it ...BeehiveBy beehive.govt.nz1 week ago
President Adeang, fellow Ministers, honourable Diet Member Horii, Ambassadors, distinguished guests. Minasama, konnichiwa, and good afternoon, everyone. Distinguished guests, it’s a pleasure to be here with you today to talk about New Zealand’s foreign policy reset, the reasons for it, the values that underpin it, and how it ...BeehiveBy beehive.govt.nz1 week ago
Related Posts
- 'Enough is enough' – Chris Hipkins blasts government over Māori policies
 Labour Party leader Chris Hipkins says the coalition government is unfairly targeting Māori: "Each week they find new ways to keep Māori down." ...48 mins ago
Labour Party leader Chris Hipkins says the coalition government is unfairly targeting Māori: "Each week they find new ways to keep Māori down." ...48 mins ago - Focus on Politics: Abuse in care report delivers demands for justice
 The government has promised to listen to survivors, but how it responds and whether justice is served remains to be seen. ...6 hours ago
The government has promised to listen to survivors, but how it responds and whether justice is served remains to be seen. ...6 hours ago - Green AGM: Party processes will be respected on Darleen Tana issue, Chlöe Swarbrick says
 A Green Party member is concerned that proper process will not be followed - but the party's co-leader says a vote will not be forced. ...6 hours ago
A Green Party member is concerned that proper process will not be followed - but the party's co-leader says a vote will not be forced. ...6 hours ago - Short story: Fire Engines, by Gina Butson
 Last summer when Matairangi burned, Ginny and Tom stood at the window of their lounge, watching kākā shoot skyward from the burning trees. From the distance, they looked to Ginny like pages torn from books and thrown into a bonfire. It was Tom, voice tight, who told her it was ...NewsroomBy Gina Butson6 hours ago
Last summer when Matairangi burned, Ginny and Tom stood at the window of their lounge, watching kākā shoot skyward from the burning trees. From the distance, they looked to Ginny like pages torn from books and thrown into a bonfire. It was Tom, voice tight, who told her it was ...NewsroomBy Gina Butson6 hours ago - Alice Munro’s shocking silence
 Opinion: The Canadian short story writer Alice Munro – winner of the Nobel Prize in Literature in 2013 – died in May at the age of 92. Her work was about “the damage people inflict on one another in the name of love”, Deborah Treisman wrote in the New Yorker. ...NewsroomBy Dr Paula Morris6 hours ago
Opinion: The Canadian short story writer Alice Munro – winner of the Nobel Prize in Literature in 2013 – died in May at the age of 92. Her work was about “the damage people inflict on one another in the name of love”, Deborah Treisman wrote in the New Yorker. ...NewsroomBy Dr Paula Morris6 hours ago - Re-writing the timeline of the universe
 This month marks two years since the most powerful telescope ever built sent its first pictures back to earth. From its lofty vantage point, beyond the moon in orbit around the sun, the James Webb Space Telescope was tuned to observe the first stars and galaxies being born soon after ...NewsroomBy The Detail contributor6 hours ago
This month marks two years since the most powerful telescope ever built sent its first pictures back to earth. From its lofty vantage point, beyond the moon in orbit around the sun, the James Webb Space Telescope was tuned to observe the first stars and galaxies being born soon after ...NewsroomBy The Detail contributor6 hours ago - Anne Salmond: What track was that?
 Comment: After Climate Change Minister Simon Watts’ preview several weeks ago, I had some optimism about the Government’s emissions reduction plan. Now I’ve read the discussion document, that hope has been dashed. How can the Government propose a plan that wants to take New Zealand taxpayers’ hard-earned money, and spend ...NewsroomBy Dame Anne Salmond6 hours ago
Comment: After Climate Change Minister Simon Watts’ preview several weeks ago, I had some optimism about the Government’s emissions reduction plan. Now I’ve read the discussion document, that hope has been dashed. How can the Government propose a plan that wants to take New Zealand taxpayers’ hard-earned money, and spend ...NewsroomBy Dame Anne Salmond6 hours ago - The Secret Diary of .. NZ’s Olympics hopefuls
 Christopher Luxon: hurdles The little man from National jumps hurdles in his sleep. He’s quite good at it in his dreams and even though the reality doesn’t quite match up you have to give him credit for getting up every morning and crashing into the very first hurdle of the ...NewsroomBy Steve Braunias6 hours ago
Christopher Luxon: hurdles The little man from National jumps hurdles in his sleep. He’s quite good at it in his dreams and even though the reality doesn’t quite match up you have to give him credit for getting up every morning and crashing into the very first hurdle of the ...NewsroomBy Steve Braunias6 hours ago - Finally heard, seen – and believed
 Comment: It was a good two hours into the conversation when Tyrone Marks raised the most basic of questions when I first spoke to him in 2017. “They didn’t explain the things they did to me. They never told me why. And they still haven’t. There’s no explanation for it. ...NewsroomBy Aaron Smale6 hours ago
Comment: It was a good two hours into the conversation when Tyrone Marks raised the most basic of questions when I first spoke to him in 2017. “They didn’t explain the things they did to me. They never told me why. And they still haven’t. There’s no explanation for it. ...NewsroomBy Aaron Smale6 hours ago - The Weekend: If in doubt, go to the funeral
 Madeleine Chapman rounds out Death Week on The Spinoff with a final recommendation. You can read all of our Death Week coverage here. Nothing forces you to reflect on your life and relationships quite like proximity to death. For those whose nearest and dearest have died, there are reasonably obvious ...The SpinoffBy Madeleine Chapman7 hours ago
Madeleine Chapman rounds out Death Week on The Spinoff with a final recommendation. You can read all of our Death Week coverage here. Nothing forces you to reflect on your life and relationships quite like proximity to death. For those whose nearest and dearest have died, there are reasonably obvious ...The SpinoffBy Madeleine Chapman7 hours ago - ‘What a privilege’: Whitney from The Traitors NZ on life as a funeral director
 Whitney Greene takes us through her life in television, including the TV character she’d like to plan a funeral for and her cow lung catastrophe on The Traitors NZ. “If the phone rings, I have to answer it,” Whitney Greene from The Traitors NZ warns as we begin our My ...The SpinoffBy My Life in TV7 hours ago
Whitney Greene takes us through her life in television, including the TV character she’d like to plan a funeral for and her cow lung catastrophe on The Traitors NZ. “If the phone rings, I have to answer it,” Whitney Greene from The Traitors NZ warns as we begin our My ...The SpinoffBy My Life in TV7 hours ago - Rich and rare: Bad Archive by Flora Feltham, reviewed
 Maddie Ballard reviews the debut essay collection of Pōneke writer Flora Feltham. In ‘The Raw Material’, the longest essay in Flora Feltham’s dazzling debut collection, the author heads out for a run after hours of weaving and sees the world turn to textile. “Pounding along the Parade, I saw the ...The SpinoffBy Maddie Ballard7 hours ago
Maddie Ballard reviews the debut essay collection of Pōneke writer Flora Feltham. In ‘The Raw Material’, the longest essay in Flora Feltham’s dazzling debut collection, the author heads out for a run after hours of weaving and sees the world turn to textile. “Pounding along the Parade, I saw the ...The SpinoffBy Maddie Ballard7 hours ago - ‘Possibly the best live gig I have been to’: TRiPS’ perfect weekend playlist
 Andy Christiansen, one half of the experimental rock-pop duo TRiPS, shares the tunes inspiring the band’s perfect weekend and new release. “Good speakers, good food, good music, no distractions”: that’s all you need to enjoy the psychedelic stylings of TRiPS, a new band formed by Fly My Pretties’ Barnaby Weir ...The SpinoffBy Weekend playlist7 hours ago
Andy Christiansen, one half of the experimental rock-pop duo TRiPS, shares the tunes inspiring the band’s perfect weekend and new release. “Good speakers, good food, good music, no distractions”: that’s all you need to enjoy the psychedelic stylings of TRiPS, a new band formed by Fly My Pretties’ Barnaby Weir ...The SpinoffBy Weekend playlist7 hours ago - Every sport at the Paris Olympics, ranked from least to most fun to watch
 Celebrating our quadrennial opportunity to become experts in a bunch of sports we never normally watch. The games of the XXXIII Olympiad are upon us. Paris will host this year’s showcase of sporting and athletic prowess, which means some late-night and early-morning viewing for us in Aotearoa. But what sports ...The SpinoffBy Mathew Nash7 hours ago
Celebrating our quadrennial opportunity to become experts in a bunch of sports we never normally watch. The games of the XXXIII Olympiad are upon us. Paris will host this year’s showcase of sporting and athletic prowess, which means some late-night and early-morning viewing for us in Aotearoa. But what sports ...The SpinoffBy Mathew Nash7 hours ago - The Sunday Essay: Remembering my brother
 The photograph is striking and beautiful, but also disturbing – a reminder that my love for John was often entangled in shame. The Sunday Essay is made possible thanks to the support of Creative New Zealand. In the spring of 1980, in Dunedin, shortly before his death, someone took a photograph ...The SpinoffBy Dougal Rillstone7 hours ago
The photograph is striking and beautiful, but also disturbing – a reminder that my love for John was often entangled in shame. The Sunday Essay is made possible thanks to the support of Creative New Zealand. In the spring of 1980, in Dunedin, shortly before his death, someone took a photograph ...The SpinoffBy Dougal Rillstone7 hours ago - Dog of the month: Babushka, who is notorious in Newtown
 Get to know Babushka, our latest Dog of the Month. This feature was offered as a reward during our What’s Eating Aotearoa PledgeMe campaign. Thank you to Babu’s humans, Jo and Isabel, for their support. Dog name: Babushka (Babu for short) Age: 2 Breed: Border Collie X poodle If rescued, ...The SpinoffBy The Spinoff7 hours ago
Get to know Babushka, our latest Dog of the Month. This feature was offered as a reward during our What’s Eating Aotearoa PledgeMe campaign. Thank you to Babu’s humans, Jo and Isabel, for their support. Dog name: Babushka (Babu for short) Age: 2 Breed: Border Collie X poodle If rescued, ...The SpinoffBy The Spinoff7 hours ago - Photojournalist targeted by Israeli army carries Olympic torch in Paris
 Pacific Media Watch A Lebanese photojournalist who was severely wounded during an Israeli air strike in south Lebanon carried the Olympic torch in Paris this week in honour of her peers who have been wounded and killed in the field — especially in Gaza and Lebanon. Christina Assi of Agence ...Evening ReportBy Asia Pacific Report14 hours ago
Pacific Media Watch A Lebanese photojournalist who was severely wounded during an Israeli air strike in south Lebanon carried the Olympic torch in Paris this week in honour of her peers who have been wounded and killed in the field — especially in Gaza and Lebanon. Christina Assi of Agence ...Evening ReportBy Asia Pacific Report14 hours ago - 70 years on from tests, Marshallese women still fight for nuclear justice
 The first report in a five-part web series focused on the 15th Triennial Conference of Pacific Women taking place in the Marshall Islands this week. SPECIAL REPORT: By Netani Rika in Majuro Women continue to fight for justice 70 years after the first nuclear tests by the United States caused ...Evening ReportBy Asia Pacific Report15 hours ago
The first report in a five-part web series focused on the 15th Triennial Conference of Pacific Women taking place in the Marshall Islands this week. SPECIAL REPORT: By Netani Rika in Majuro Women continue to fight for justice 70 years after the first nuclear tests by the United States caused ...Evening ReportBy Asia Pacific Report15 hours ago - 'Israel must listen' – Luxon, Albanese, Trudeau issue joint support for US-backed ce...
 Christopher Luxon has joined with Australia and Canada's leaders in voicing support for US President Joe Biden's ceasefire deal between Israel and Hamas. ...16 hours ago
Christopher Luxon has joined with Australia and Canada's leaders in voicing support for US President Joe Biden's ceasefire deal between Israel and Hamas. ...16 hours ago - Politics with Michelle Grattan: ‘Teal’ Zoe Daniel on political donations, representing Jewish vo...
 Source: The Conversation (Au and NZ) – By Michelle Grattan, Professorial Fellow, University of Canberra The 2022 election brought the “teal wave” into parliament. The next election will test whether teals, who occupy what were Liberal seats, and other independents can maintain their momentum. Joining us on the Podcast ...Evening ReportBy The Conversation16 hours ago
Source: The Conversation (Au and NZ) – By Michelle Grattan, Professorial Fellow, University of Canberra The 2022 election brought the “teal wave” into parliament. The next election will test whether teals, who occupy what were Liberal seats, and other independents can maintain their momentum. Joining us on the Podcast ...Evening ReportBy The Conversation16 hours ago - China: still the world’s biggest emitter, but also an emerging force in climate diplomacy
 Source: The Conversation (Au and NZ) – By Xu Yi-chong, Professor of Governance and Public Policy, Griffith University fuyu liu, Shutterstock Seven years seems a lifetime in politics. In 2017, President Donald Trump announced the United States would withdraw from the Paris Agreement. It prompted Canada, China and the ...Evening ReportBy The Conversation16 hours ago
Source: The Conversation (Au and NZ) – By Xu Yi-chong, Professor of Governance and Public Policy, Griffith University fuyu liu, Shutterstock Seven years seems a lifetime in politics. In 2017, President Donald Trump announced the United States would withdraw from the Paris Agreement. It prompted Canada, China and the ...Evening ReportBy The Conversation16 hours ago - Federal Court finds insufficient evidence Roundup weedkiller causes cancer. What does the science sa...
 Source: The Conversation (Au and NZ) – By Ian Musgrave, Senior lecturer in Pharmacology, University of Adelaide Pixavri/Shutterstock A major Federal Court class action has been dismissed this week after Justice Michael Lee ruled there was not enough evidence to prove the weedkiller Roundup causes cancer. Plaintiff Kelvin ...Evening ReportBy The Conversation17 hours ago
Source: The Conversation (Au and NZ) – By Ian Musgrave, Senior lecturer in Pharmacology, University of Adelaide Pixavri/Shutterstock A major Federal Court class action has been dismissed this week after Justice Michael Lee ruled there was not enough evidence to prove the weedkiller Roundup causes cancer. Plaintiff Kelvin ...Evening ReportBy The Conversation17 hours ago - The Week in Politics: Parliament set a vital task, Darleen Tana returns
 In The Week in Politics: politicians have to decide what to do about child abuse, Health NZ is booked in for major surgery and Darleen Tana returns. ...17 hours ago
In The Week in Politics: politicians have to decide what to do about child abuse, Health NZ is booked in for major surgery and Darleen Tana returns. ...17 hours ago - Māori leader says government's controversial boot camps the wrong approach
18 hours ago
- Twice as good for half the respect: Kamala Harris’ battle for the White House
 Source: The Conversation (Au and NZ) – By Clare Corbould, Associate Professor, Contemporary Histories Research Group, Deakin University Mainstream media are surprisingly muted at the prospect of the world’s most powerful nation being led for the first time by a woman – specifically a woman of colour, Vice President Kamala ...Evening ReportBy The Conversation18 hours ago
Source: The Conversation (Au and NZ) – By Clare Corbould, Associate Professor, Contemporary Histories Research Group, Deakin University Mainstream media are surprisingly muted at the prospect of the world’s most powerful nation being led for the first time by a woman – specifically a woman of colour, Vice President Kamala ...Evening ReportBy The Conversation18 hours ago - Drone food delivery is spreading across Australia. Research suggests we will eat more junk food as a...
 Source: The Conversation (Au and NZ) – By Rebecca Bennett, PhD Student, Associate Research Fellow, Deakin University Last week, a drone delivery company called Wing (owned by Google’s parent company, Alphabet) started operating in Melbourne. Some 250,000 residents in parts of the city’s eastern suburbs can now order food from ...Evening ReportBy The Conversation18 hours ago
Source: The Conversation (Au and NZ) – By Rebecca Bennett, PhD Student, Associate Research Fellow, Deakin University Last week, a drone delivery company called Wing (owned by Google’s parent company, Alphabet) started operating in Melbourne. Some 250,000 residents in parts of the city’s eastern suburbs can now order food from ...Evening ReportBy The Conversation18 hours ago - Our research shows 4 in 10 Australians in aged care are malnourished. What can we do about it?
 Source: The Conversation (Au and NZ) – By Jonathan Foo, Lecturer, Physiotherapy, Monash University pikselstock/Shutterstock In the next 40 years in Australia, it’s predicted the number of Australians aged 65 and over will more than double, while the number of people aged 85 and over will more than triple. ...Evening ReportBy The Conversation18 hours ago
Source: The Conversation (Au and NZ) – By Jonathan Foo, Lecturer, Physiotherapy, Monash University pikselstock/Shutterstock In the next 40 years in Australia, it’s predicted the number of Australians aged 65 and over will more than double, while the number of people aged 85 and over will more than triple. ...Evening ReportBy The Conversation18 hours ago - Before there was diving and relays, there was the Poetry Olympics
 Source: The Conversation (Au and NZ) – By Katrina Grant, Research Associate, Power Institute for Arts and Visual Culture, University of Sydney Jonas Åkerström’s 1790 work, Session of the Accademia dell’Arcadia on August 17 1788. Nationalmuseum/Cecilia Heisser Ever wondered whether you’d have a better chance at winning an Olympic gold ...Evening ReportBy The Conversation19 hours ago
Source: The Conversation (Au and NZ) – By Katrina Grant, Research Associate, Power Institute for Arts and Visual Culture, University of Sydney Jonas Åkerström’s 1790 work, Session of the Accademia dell’Arcadia on August 17 1788. Nationalmuseum/Cecilia Heisser Ever wondered whether you’d have a better chance at winning an Olympic gold ...Evening ReportBy The Conversation19 hours ago - Abuse in Care inquiry: Judith Collins warns of possible prosecutions if records destroyed
 Judith Collins is reminding all state and faith-based institutions of their legal obligation to preserve records. ...19 hours ago
Judith Collins is reminding all state and faith-based institutions of their legal obligation to preserve records. ...19 hours ago - Health star labels move closer to being mandatory. But food companies could still (legally) game the...
 Source: The Conversation (Au and NZ) – By Alexandra Jones, Program Lead, Food Governance, George Institute for Global Health wavebreakmedia/Shutterstock On Thursday, Australian and New Zealand food ministers at state, federal and national levels met to thrash out what’s next for health star ratings on packaged foods. Now, after ...Evening ReportBy The Conversation20 hours ago
Source: The Conversation (Au and NZ) – By Alexandra Jones, Program Lead, Food Governance, George Institute for Global Health wavebreakmedia/Shutterstock On Thursday, Australian and New Zealand food ministers at state, federal and national levels met to thrash out what’s next for health star ratings on packaged foods. Now, after ...Evening ReportBy The Conversation20 hours ago - Abuse in Care inquiry: Call for Pacific focused redress pathway
 The Abuse in Care report found many Pacific survivors lost their connections to their culture and language, resulting in trauma that has been carried from generation to generation. ...20 hours ago
The Abuse in Care report found many Pacific survivors lost their connections to their culture and language, resulting in trauma that has been carried from generation to generation. ...20 hours ago - Education Review Office Pragmatism Will Really Help The Sector While The Regulation Review Is Underw...
 In the regulatory review, ECC intends to suggest that ERO focus on curriculum delivery reviews rather than the Ministry, because it’s not efficient or effective to have two agencies with radically different approaches climbing over each other. ...21 hours ago
In the regulatory review, ECC intends to suggest that ERO focus on curriculum delivery reviews rather than the Ministry, because it’s not efficient or effective to have two agencies with radically different approaches climbing over each other. ...21 hours ago - Watch: Christopher Luxon's security cut short visit ahead of protest
 The prime minister was speaking to reporters during a walkabout with police in central Auckland. ...21 hours ago
The prime minister was speaking to reporters during a walkabout with police in central Auckland. ...21 hours ago - Christopher Luxon calls for witnesses to alleged '80s politician paedophile ring to speak out
 Christopher Luxon says anyone with evidence about claims involving politicians and civil servants in the 1980s should go to police. ...22 hours ago
Christopher Luxon says anyone with evidence about claims involving politicians and civil servants in the 1980s should go to police. ...22 hours ago - Co-chairs Of Te Rūnanga Nui O Ngā Kura Kaupapa Māori Welcome The Waitangi Tribunal Report –...
 Te Rūnanga Nui o Ngā Kura Kaupapa Māori invites the current government to work in partnership with them to develop a pathway forward, including the development of a parallel pathway and meaningful policy and strategy for Kura Kaupapa Māori ...22 hours ago
Te Rūnanga Nui o Ngā Kura Kaupapa Māori invites the current government to work in partnership with them to develop a pathway forward, including the development of a parallel pathway and meaningful policy and strategy for Kura Kaupapa Māori ...22 hours ago - Why this season of The Traitors is the best reality TV NZ has ever made
 If you haven’t started watching yet, Tara Ward begs you to reconsider. This is an excerpt from our weekly pop culture newsletter Rec Room. Sign up here. In the world of New Zealand reality television, we have many gems in our crown. There’s the delicious second season of the Celebrity Treasure ...The SpinoffBy Tara Ward22 hours ago
If you haven’t started watching yet, Tara Ward begs you to reconsider. This is an excerpt from our weekly pop culture newsletter Rec Room. Sign up here. In the world of New Zealand reality television, we have many gems in our crown. There’s the delicious second season of the Celebrity Treasure ...The SpinoffBy Tara Ward22 hours ago - The Friday Poem: ‘The clothes of the dead’ by Fiona Kidman
 A new poem by Fiona Kidman. The clothes of the dead I did not keep my mother’s furry red beret for long nor the stringy scarves that adorned the necks of my aunts, although I have kept tag ends of gold, the rings and trinkets they wore, the brooches no ...The SpinoffBy Fiona Kidman22 hours ago
A new poem by Fiona Kidman. The clothes of the dead I did not keep my mother’s furry red beret for long nor the stringy scarves that adorned the necks of my aunts, although I have kept tag ends of gold, the rings and trinkets they wore, the brooches no ...The SpinoffBy Fiona Kidman22 hours ago - Ngāi Tahu Challenges Changes To MACA
 The government’s announcement that it will re-open the foreshore and seabed controversy by changing the rules on recognising centuries-old Māori customary title for a third time goes against the rule of law and New Zealand values,” Mr Tipa says. ...22 hours ago
The government’s announcement that it will re-open the foreshore and seabed controversy by changing the rules on recognising centuries-old Māori customary title for a third time goes against the rule of law and New Zealand values,” Mr Tipa says. ...22 hours ago - The Unity Books bestseller chart for the week ending July 26
 The only published and available best-selling indie book chart in New Zealand is the top 10 sales list recorded every week at Unity Books’ stores in High St, Auckland, and Willis St, Wellington. AUCKLAND 1 Lioness by Emily Perkins (Bloomsbury, $25) Roarrrr! Perkins’ brilliant, award-winning, Marian-Keyes anointed, darkly funny, long ...The SpinoffBy The Spinoff Review of Books22 hours ago
The only published and available best-selling indie book chart in New Zealand is the top 10 sales list recorded every week at Unity Books’ stores in High St, Auckland, and Willis St, Wellington. AUCKLAND 1 Lioness by Emily Perkins (Bloomsbury, $25) Roarrrr! Perkins’ brilliant, award-winning, Marian-Keyes anointed, darkly funny, long ...The SpinoffBy The Spinoff Review of Books22 hours ago - Overturning Court Of Appeal Decision On Foreshore And Seabed Is Abuse Of Power
 The 2004 Act vested ownership of the foreshore and seabed in the Crown, extinguishing any Māori claims to ownership and causing widespread outrage and protests among Māori communities. ...22 hours ago
The 2004 Act vested ownership of the foreshore and seabed in the Crown, extinguishing any Māori claims to ownership and causing widespread outrage and protests among Māori communities. ...22 hours ago - Gang crackdown: why anti-patch policies backfire – and what would actually work
 Source: The Conversation (Au and NZ) – By Antje Deckert, Associate Professor (Criminology), Auckland University of Technology Getty Images Despite the connection between institutional harm and gang membership made clear in this week’s mammoth royal commission abuse-in care report, the government seems unlikely to soften its “get tough on ...Evening ReportBy The Conversation22 hours ago
Source: The Conversation (Au and NZ) – By Antje Deckert, Associate Professor (Criminology), Auckland University of Technology Getty Images Despite the connection between institutional harm and gang membership made clear in this week’s mammoth royal commission abuse-in care report, the government seems unlikely to soften its “get tough on ...Evening ReportBy The Conversation22 hours ago - Watch: Christopher Luxon's security cut short visit short ahead of protest
 The prime minister was speaking to reporters during a walkabout with police in central Auckland. ...23 hours ago
The prime minister was speaking to reporters during a walkabout with police in central Auckland. ...23 hours ago - Overruling court on coastal rights risks new protests, Te Pāti Māori warns
 Te Pāti Māori is warning a move to overturn a court decision risks a return of the big foreshore and seabed protests of 20 years ago. ...23 hours ago
Te Pāti Māori is warning a move to overturn a court decision risks a return of the big foreshore and seabed protests of 20 years ago. ...23 hours ago - New Zealanders in action: When and who to watch in week one of the Paris Olympics
 From Lewis Clareburt in the swimming to the start of the rowing – the first seven days of Paris 2024 promise to be big for New Zealand. There are few events that bring the country together quite like an Olympic Games. Nothing quite matches the excitement of getting up in ...The SpinoffBy Stewart Sowman-Lund23 hours ago
From Lewis Clareburt in the swimming to the start of the rowing – the first seven days of Paris 2024 promise to be big for New Zealand. There are few events that bring the country together quite like an Olympic Games. Nothing quite matches the excitement of getting up in ...The SpinoffBy Stewart Sowman-Lund23 hours ago - The local science that just made a huge cameo in The Kardashians
 Groundbreaking local science just showed up in the most surprising of places: the season finale of The Kardashians. In the season five finale of The Kardashians last night, several members of the family gathered together in one of their signature empty, cream-coloured rooms to hear test results that had been ...The SpinoffBy Alex Casey23 hours ago
Groundbreaking local science just showed up in the most surprising of places: the season finale of The Kardashians. In the season five finale of The Kardashians last night, several members of the family gathered together in one of their signature empty, cream-coloured rooms to hear test results that had been ...The SpinoffBy Alex Casey23 hours ago - Can Israel and Hezbollah be pulled back from the brink of war?
 Source: The Conversation (Au and NZ) – By Amin Saikal, Emeritus professor of Middle Eastern and Central Asian Studies, Australian National University The Middle East is on the brink of a possibly devastating regional war, with hostilities between Israel and Hezbollah reaching an extremely dangerous level. Washington has engaged in ...Evening ReportBy The Conversation23 hours ago
Source: The Conversation (Au and NZ) – By Amin Saikal, Emeritus professor of Middle Eastern and Central Asian Studies, Australian National University The Middle East is on the brink of a possibly devastating regional war, with hostilities between Israel and Hezbollah reaching an extremely dangerous level. Washington has engaged in ...Evening ReportBy The Conversation23 hours ago - Lupus is more common and severe in Aboriginal and Torres Strait Islander peoples. Learning why is cr...
 Source: The Conversation (Au and NZ) – By Laura Elizabeth Eades, Rheumatologist, Monash University Lupus is an inflammatory autoimmune illness, where the body’s immune system mistakenly attacks itself. Lupus can affect virtually any part of the body, although it most commonly affects the skin, joints and kidneys. The symptoms ...Evening ReportBy The Conversation23 hours ago
Source: The Conversation (Au and NZ) – By Laura Elizabeth Eades, Rheumatologist, Monash University Lupus is an inflammatory autoimmune illness, where the body’s immune system mistakenly attacks itself. Lupus can affect virtually any part of the body, although it most commonly affects the skin, joints and kidneys. The symptoms ...Evening ReportBy The Conversation23 hours ago - Government Fails To Recognise Parallels Between Whakapakari And Its Boot Camps
 A law firm that specialises in working with survivors of abuse in State care is disappointed that the Government fails to recognise that its boot camps can be directly compared to previous boot camps from the 1990s and 2000s. ...24 hours ago
A law firm that specialises in working with survivors of abuse in State care is disappointed that the Government fails to recognise that its boot camps can be directly compared to previous boot camps from the 1990s and 2000s. ...24 hours ago - Crown breached Treaty principles in school reform – Waitangi Tribunal
 A Waitangi Tribunal report has found the Crown breached Treaty principles in its review and reform of schools between 2018 and 2022. ...24 hours ago
A Waitangi Tribunal report has found the Crown breached Treaty principles in its review and reform of schools between 2018 and 2022. ...24 hours ago - Zero stars: Rating the experience of death and dying in Aotearoa
 Dying is a natural part of life, like updating your Wof or seeing your hairdresser, but without the word-of-mouth recs that help guarantee a good service. What if we changed that? Dying Reviews received by The Spinoff have had the names of organisations redacted while Hospice NZ collects further data. ...The SpinoffBy Lyric Waiwiri-Smith24 hours ago
Dying is a natural part of life, like updating your Wof or seeing your hairdresser, but without the word-of-mouth recs that help guarantee a good service. What if we changed that? Dying Reviews received by The Spinoff have had the names of organisations redacted while Hospice NZ collects further data. ...The SpinoffBy Lyric Waiwiri-Smith24 hours ago - Not one, but two meteor showers are about to peak – here’s how to catch the stellar show
 Source: The Conversation (Au and NZ) – By Jonti Horner, Professor (Astrophysics), University of Southern Queensland Mike Lewinski/Flickr, CC BY On any clear night, if you gaze skywards long enough, chances are you’ll see a meteor streaking through the sky. Some nights, however, are better than others. At ...Evening ReportBy The Conversation1 day ago
Source: The Conversation (Au and NZ) – By Jonti Horner, Professor (Astrophysics), University of Southern Queensland Mike Lewinski/Flickr, CC BY On any clear night, if you gaze skywards long enough, chances are you’ll see a meteor streaking through the sky. Some nights, however, are better than others. At ...Evening ReportBy The Conversation1 day ago - Ministry of Education puts 100 school building projects on ice
1 day ago
- How Tāmaki Makaurau became home to the world’s only lesbian museum
 Despite having no bars or other designated spaces for lesbians, Auckland boasts a small but mighty lesbian museum. So how did it get here? The past 18 months has brought increasing hostility towards the queer community across Aotearoa. Kellie-Jay Keen-Minshull’s anti-trans rally in Tamaki Makaurau last March led to a ...The SpinoffBy Kitty Wasasala1 day ago
Despite having no bars or other designated spaces for lesbians, Auckland boasts a small but mighty lesbian museum. So how did it get here? The past 18 months has brought increasing hostility towards the queer community across Aotearoa. Kellie-Jay Keen-Minshull’s anti-trans rally in Tamaki Makaurau last March led to a ...The SpinoffBy Kitty Wasasala1 day ago - Protest At French Embassy Calls Out Hypocrisy In Kanaky As Paris Olympics Begin
 Poneke Antifascist Coalition has invited Wellingtonians to stand in solidarity with the Kanak people at 12pm today outside the French Embassy in Wellington. ...1 day ago
Poneke Antifascist Coalition has invited Wellingtonians to stand in solidarity with the Kanak people at 12pm today outside the French Embassy in Wellington. ...1 day ago - Chicken wire, AI and mobile phones on sticks: how the drone war in Ukraine is driving a fierce battl...
 Source: The Conversation (Au and NZ) – By Peter Layton, Visiting Fellow, Strategic Studies, Griffith University Drones are the signature technology of the Ukraine war. A few miniature aircraft designs were used in the war’s early days, but an incredible array of drones have now evolved. There are different types, ...Evening ReportBy The Conversation1 day ago
Source: The Conversation (Au and NZ) – By Peter Layton, Visiting Fellow, Strategic Studies, Griffith University Drones are the signature technology of the Ukraine war. A few miniature aircraft designs were used in the war’s early days, but an incredible array of drones have now evolved. There are different types, ...Evening ReportBy The Conversation1 day ago - What happens in my brain when I get a migraine? And what medications can I use to treat it?
 Source: The Conversation (Au and NZ) – By Mark Slee, Associate Professor, Clinical Academic Neurologist, Flinders University Francisco Gonzelez/Unsplash Migraine is many things, but one thing it’s not is “just a headache”. “Migraine” comes from the Greek word “hemicrania”, referring to the common experience of migraine being predominantly ...Evening ReportBy The Conversation1 day ago
Source: The Conversation (Au and NZ) – By Mark Slee, Associate Professor, Clinical Academic Neurologist, Flinders University Francisco Gonzelez/Unsplash Migraine is many things, but one thing it’s not is “just a headache”. “Migraine” comes from the Greek word “hemicrania”, referring to the common experience of migraine being predominantly ...Evening ReportBy The Conversation1 day ago - How old, inefficient housing and time-of-use electricity rates are leaving some households worse off
 Source: The Conversation (Au and NZ) – By Lee White, Senior Lecturer and Horizon Fellow, School of Social and Political Sciences, University of Sydney Australia was slow to introduce minimum building standards for energy efficiency. The Nationwide House Energy Rating Scheme (NatHERS) only came into force in 2003. Older homes ...Evening ReportBy The Conversation1 day ago
Source: The Conversation (Au and NZ) – By Lee White, Senior Lecturer and Horizon Fellow, School of Social and Political Sciences, University of Sydney Australia was slow to introduce minimum building standards for energy efficiency. The Nationwide House Energy Rating Scheme (NatHERS) only came into force in 2003. Older homes ...Evening ReportBy The Conversation1 day ago - Landmark new research shows how global warming is messing with our rainfall
 Source: The Conversation (Au and NZ) – By Steven Sherwood, Professor of Atmospheric Sciences, Climate Change Research Centre, UNSW Sydney The past century of human-induced warming has increased rainfall variability over 75% of the Earth’s land area – particularly over Australia, Europe and eastern North America, new research shows. ...Evening ReportBy The Conversation1 day ago
Source: The Conversation (Au and NZ) – By Steven Sherwood, Professor of Atmospheric Sciences, Climate Change Research Centre, UNSW Sydney The past century of human-induced warming has increased rainfall variability over 75% of the Earth’s land area – particularly over Australia, Europe and eastern North America, new research shows. ...Evening ReportBy The Conversation1 day ago - Timber venues, river swimming and re-use: how the Paris Olympics is going green – and what it’s ...
 Source: The Conversation (Au and NZ) – By Tony Heynen, Program Coordinator, Sustainable Energy, The University of Queensland A temporary stadium in the Champ-de-Mars, Paris Ekaterina Pokrovsky/Shutterstock As Paris prepares to host the Olympic and Paralympic Games, the sustainability of the event is coming under scrutiny. The organisers have promoted ...Evening ReportBy The Conversation1 day ago
Source: The Conversation (Au and NZ) – By Tony Heynen, Program Coordinator, Sustainable Energy, The University of Queensland A temporary stadium in the Champ-de-Mars, Paris Ekaterina Pokrovsky/Shutterstock As Paris prepares to host the Olympic and Paralympic Games, the sustainability of the event is coming under scrutiny. The organisers have promoted ...Evening ReportBy The Conversation1 day ago - An Ode to Newtown Sports Bar, Wellington’s last great pub
 A night of karaoke and community in a pub that feels like a memory. You’d barely even notice it, unless you knew to look. Tucked away behind a liquor store on busy Constable Street is the capital’s last great pub. Newtown Sports Bar is an emblem of the pub culture ...The SpinoffBy Henessey Griffiths1 day ago
A night of karaoke and community in a pub that feels like a memory. You’d barely even notice it, unless you knew to look. Tucked away behind a liquor store on busy Constable Street is the capital’s last great pub. Newtown Sports Bar is an emblem of the pub culture ...The SpinoffBy Henessey Griffiths1 day ago - Health commissioner in meetings over new Dunedin Hospital cost blowout
 The spotlight will then turn on the proposed new regional hospitals for Nelson, Hawke’s Bay, Tauranga and Palmerston North The post Health commissioner in meetings over new Dunedin Hospital cost blowout appeared first on Newsroom. ...NewsroomBy Jonathan Milne1 day ago
The spotlight will then turn on the proposed new regional hospitals for Nelson, Hawke’s Bay, Tauranga and Palmerston North The post Health commissioner in meetings over new Dunedin Hospital cost blowout appeared first on Newsroom. ...NewsroomBy Jonathan Milne1 day ago - Declining PhD student numbers are a warning sign for NZ’s future knowledge economy
 Source: The Conversation (Au and NZ) – By Ian Wright, Professor in Marine Geology, University of Canterbury Louise Corcoran/Getty Images The decline in the number of doctoral candidates at New Zealand universities is a worrying sign for the country’s effort to build a knowledge-based economy. Aotearoa New Zealand’s ...Evening ReportBy The Conversation1 day ago
Source: The Conversation (Au and NZ) – By Ian Wright, Professor in Marine Geology, University of Canterbury Louise Corcoran/Getty Images The decline in the number of doctoral candidates at New Zealand universities is a worrying sign for the country’s effort to build a knowledge-based economy. Aotearoa New Zealand’s ...Evening ReportBy The Conversation1 day ago - Migrant workers have long been too scared to report employer misconduct. A new visa could change thi...
 Source: The Conversation (Au and NZ) – By Laurie Berg, Associate Professor, University of Technology Sydney defotoberg/Shutterstock Migrant worker exploitation is entrenched in workplaces across Australia. Tragically, a deep fear of immigration consequences means most unlawful employer conduct goes unreported. On Wednesday, however, the government officially launched a ...Evening ReportBy The Conversation1 day ago
Source: The Conversation (Au and NZ) – By Laurie Berg, Associate Professor, University of Technology Sydney defotoberg/Shutterstock Migrant worker exploitation is entrenched in workplaces across Australia. Tragically, a deep fear of immigration consequences means most unlawful employer conduct goes unreported. On Wednesday, however, the government officially launched a ...Evening ReportBy The Conversation1 day ago - The chaotic history of the Olympics in Paris, where one games nearly ended the movement – and the ...
 Source: The Conversation (Au and NZ) – By Vaughan Cruickshank, Senior Lecturer in Health and Physical Education, University of Tasmania Paris is about to host its third summer Olympics. While we don’t yet know what the legacy of this year’s games will be, let’s take the opportunity to reflect on ...Evening ReportBy The Conversation1 day ago
Source: The Conversation (Au and NZ) – By Vaughan Cruickshank, Senior Lecturer in Health and Physical Education, University of Tasmania Paris is about to host its third summer Olympics. While we don’t yet know what the legacy of this year’s games will be, let’s take the opportunity to reflect on ...Evening ReportBy The Conversation1 day ago - ‘Bloodbath’, ‘bullseye’, ‘America’s Hitler’: why has our political rhetoric gotten so ...
 Source: The Conversation (Au and NZ) – By Hugh Breakey, Deputy Director, Institute for Ethics, Governance & Law, Griffith University In the wake of the assassination attempt on former US President Donald Trump, there were calls from both sides of US politics, as well as internationally, to reduce the brutal, ...Evening ReportBy The Conversation1 day ago
Source: The Conversation (Au and NZ) – By Hugh Breakey, Deputy Director, Institute for Ethics, Governance & Law, Griffith University In the wake of the assassination attempt on former US President Donald Trump, there were calls from both sides of US politics, as well as internationally, to reduce the brutal, ...Evening ReportBy The Conversation1 day ago - Politics, security and the Seine: where the Paris Olympics’ flashpoints will be
 Source: The Conversation (Au and NZ) – By Keith Rathbone, Senior Lecturer, Modern European History and Sports History, Macquarie University Two high-profile assaults on Australians in Paris have raised concerns about security ahead of the Olympic Games. On Saturday evening, a young woman was allegedly sexually assaulted by a ...Evening ReportBy The Conversation1 day ago
Source: The Conversation (Au and NZ) – By Keith Rathbone, Senior Lecturer, Modern European History and Sports History, Macquarie University Two high-profile assaults on Australians in Paris have raised concerns about security ahead of the Olympic Games. On Saturday evening, a young woman was allegedly sexually assaulted by a ...Evening ReportBy The Conversation1 day ago - Leaked Health NZ restructure proposal shines light on latest job cuts
 There's "shock and dismay" at the health body with another "brutally fast" round of redundancies looming, one insider says. ...1 day ago
There's "shock and dismay" at the health body with another "brutally fast" round of redundancies looming, one insider says. ...1 day ago - Revisiting the cost of dying
 Dying is inevitable and, so it seems, is it costing a lot, writes Stewart Sowman-Lund in today’s extract from The Bulletin. To receive The Bulletin in full each weekday, sign up here. The cost of dying ...The SpinoffBy Stewart Sowman-Lund1 day ago
Dying is inevitable and, so it seems, is it costing a lot, writes Stewart Sowman-Lund in today’s extract from The Bulletin. To receive The Bulletin in full each weekday, sign up here. The cost of dying ...The SpinoffBy Stewart Sowman-Lund1 day ago - The state care decision that rippled through four generations
 The government took Joyce Harris's first baby and sent her off to a girls' home. Half a century on - and out of oceans of hurt - it asked her to be a mother figure. ...1 day ago
The government took Joyce Harris's first baby and sent her off to a girls' home. Half a century on - and out of oceans of hurt - it asked her to be a mother figure. ...1 day ago - Mt Victoria Tunnel, Basin Reserve plans: NZTA spent seven times more on consultants than on its own ...
 Staff working on a second Mt Victoria Tunnel and the Basin Reserve upgrade were paid $175,000 - but consultants were paid nearly $1.3 million. ...1 day ago
Staff working on a second Mt Victoria Tunnel and the Basin Reserve upgrade were paid $175,000 - but consultants were paid nearly $1.3 million. ...1 day ago - Will Gen X ever be able to retire?
 Caught between ageing parents and struggling kids, retirement planning is tough for a whole generation. ...1 day ago
Caught between ageing parents and struggling kids, retirement planning is tough for a whole generation. ...1 day ago - Minister defends lowered child poverty targets as 'achievable'
 Louise Upston has rejected criticisms of lowered child poverty reduction targets, saying they are achievable and ambitious. ...1 day ago
Louise Upston has rejected criticisms of lowered child poverty reduction targets, saying they are achievable and ambitious. ...1 day ago - What is the wildest Brokenwood Mysteries death of all time?
 It’s the deadliest fictional town in the country, but which death has been the most bonkers? Alex Casey looks back at 10 seasons of The Brokenwood Mysteries to find out. Warning: The following ranking story contains famous New Zealand actors appearing to be dead (not alive). The Spinoff has been ...The SpinoffBy Alex Casey1 day ago
It’s the deadliest fictional town in the country, but which death has been the most bonkers? Alex Casey looks back at 10 seasons of The Brokenwood Mysteries to find out. Warning: The following ranking story contains famous New Zealand actors appearing to be dead (not alive). The Spinoff has been ...The SpinoffBy Alex Casey1 day ago - ‘It’s a no-brainer’: Why Aotearoa needs to ride the wave of water cremation
 Water cremation is the biggest thing to happen to the death industry in the last 100 years. Alex Casey meets the people trying to bring it to Aotearoa. Through a set of mirrored doors down the industrial end of Christchurch’s St Asaph Street, death is getting a new lease on ...The SpinoffBy Alex Casey1 day ago
Water cremation is the biggest thing to happen to the death industry in the last 100 years. Alex Casey meets the people trying to bring it to Aotearoa. Through a set of mirrored doors down the industrial end of Christchurch’s St Asaph Street, death is getting a new lease on ...The SpinoffBy Alex Casey1 day ago - Health system must be accountable for complicity in abuse
 The tabling of the final report from the Royal Commission on Abuse in Care is a watershed moment for New Zealand. This comprehensive document lays bare the pervasive abuse and neglect experienced by children, young people, and adults in state and faith-based care from 1950 to 1999, and beyond. Among ...NewsroomBy University of Otago1 day ago
The tabling of the final report from the Royal Commission on Abuse in Care is a watershed moment for New Zealand. This comprehensive document lays bare the pervasive abuse and neglect experienced by children, young people, and adults in state and faith-based care from 1950 to 1999, and beyond. Among ...NewsroomBy University of Otago1 day ago
Related Posts
I try to read most posts here on TS and I almost always follow supplied links.
I had already, at some weird hour this morning, read the Guardian article you link to where virologist Lena Einhorn rails against the failure of the Swedish authorities to protect vulnerable residents of care facilities.
As in New Zealand, carers have been told that even basic PPE are not necessary unless the particular inmate has The Virus.
As a consequence, the death rate in this population, as here, is (to some, anyway) unacceptably high.
And the failure of the Swedish authorities to rectify this glaring fault in their Covid 19 management strategy is all the more bizarre when they claim (as does our government) that the main aim is to protect these vulnerable populations.
Thank you for adding to this conversation.
On Sweden – the glaring stat to me is that they have a low proportion of testing per million of their population. So how do they know more people haven't died but not been recorded as a C-19 death?
Exactly. And the threshold for testing here has only very recently been lowered.
I too suspect there is much wider community spread here in NZ, largely due to what we can now, with the benefit of hindsight, see was belated border controls and poor response from WHO.
I grew up in a medical household when we were all on the cusp of the vaccine rollout. The accepted wisdom was 'early and constant naturally acquired immunsation' …supported by good diet and plenty of exercise out in the fresh air and sunshine.
Part of me still thinks this makes sense as vaccines, despite the hype, are not necessarily safe or effective.
The influenza vaccine barely reaches 50% efficacy and this can lead to a false sense of security….especially in vulnerable populations who get the flu jab for free.
I worry that here in NZ there had been too much of our future thinking pinned on the hope of a vaccine…which appears less likely as time goes on.
That's why this seemingly worldwide paradox of governments claiming to have the interests of the most vulnerable at heart whilst at the same time failing to put measures in place to protect this population who require the highest levels of care.
And saying the PPE need to be conserved for future outbreaks….aren't we in the throes of an outbreak now?
Very, very baffling.
Hi Rosemary, great to get your comments.
You said:
"And the failure of the Swedish authorities to rectify this glaring fault in their Covid 19 management strategy is all the more bizarre when they claim (as does our government) that the main aim is to protect these vulnerable populations."
I feel your right, it is bizarre.
Questions
1. Do you think that across the world (and within NZ) the protection of the vulnerable has still not got to a suitable standard
2. That we (NZ) need to throw resources at this so that, so to speak the devil does not get in the door as a new study shows care homes in Europe are where over half the fatalities occur.
https://www.euronews.com/2020/04/17/coronavirus-care-homes-could-be-where-over-half-of-europe-s-covid-19-deaths-occur-says-new
3. Given potentially the current lack of PPE and capability in NZ, how would you approach making the vulnerable safe now until better capabilities arrive (how would you use your number 8 wire approach)
Take care
I have reflected on some comments yesterday on Open mike. We did all we could and within reason is the position which I feel the government needs to take. The emphasis is on "we did all we could."
To not make PPE available for home carers falls short, when it comes to the we did all we could test.
I have had years of dealings with government departments and I am still dealing with a lot of shit. All I have ever asked of them is, the we did all we could test.
I too spent time in reflection and discussion and am left with the impression that this contradictory stance by the Ministry of Health is actually part of a plan.
Sorry to say this but if this thing tracks as suspected, those uncomfortable projections done by Treasury and the like on 'long term care and fiscal sustainability ' could begin to look a lot less fiscally gloomy.
They should be transparent and say this…because I suspect a fairly high percentage of the population would would not find this too unacceptable.
Incorrect statements need to be corrected or ammended when new information is known.
It is hard to make accurate projections on care post Covid-19 due to the systemic complications of the viris, this cannot be said when it comes to being prepared with PPE for a pandemic.
Hi Treetop,
You said: "We did all we could and within reason is the position which I feel the government needs to take"
I feel your pain and agree. I don't envy the Governments task in all of this. Respectfully to the Government, we are not children, tell us the truth about our capabilities. I know there is a need to Keep Calm and Carry On, however, dont sugar coat, NZ Inc (we) are all in this together. Its surprising when Kiwis really have the problem nailed, they can come up with solutions….
Just on your point that "We did all we could", do you think we could further utilize untapped potential in our communities, universities, businesses etc….. If coordinated well it could provide alternative input to the Government. I think sometimes our GOV has a inward looking approach that uses a select few.
Image all the Universities in NZ having a competion to come up with solutions?
Be safe
I would start with untapped potential in yourself first.
What is it that I am capable of doing myself?
This is then not relying on another person. There are new skills which can be acquired gardening, sewing, painting, baking, cooking, meditation, an exercise regimen, a DIY hair cut or being the family hair stylist.
Being resilient is certainly being tested socially and economically. Most of us will manage providing we have realistic expectations and adapt to a slowed down world. Having the basics, a home, food, education, healthcare, employment or having connections is essential.
Input from the university of life, from the homeless, chronically un well and unemployed, is just as important as from university educated people.
Hi Treetop,
You said: "We did all we could and within reason is the position which I feel the government needs to take"
I feel your pain and agree. I don't envy the Governments task in all of this. Respectfully to the Government, we are not children, tell us the truth about our capabilities. I know there is a need to Keep Calm and Carry On, however, dont sugar coat, NZ Inc (we) are all in this together. Its surprising when Kiwis really have the problem nailed, they can come up with solutions….
Just on your point that "We did all we could", do you think we could further utilize untapped potential in our communities, universities, businesses etc….. If coordinated well it could provide alternative input to the Government. I think sometimes our GOV has a inward looking approach that uses a select few.
Image all the Universities in NZ having a competion to come up with solutions?
Be safe
Didn't the PM already spell out the Cabinet decision-making criteria for making the decision on Friday?
Health capacity and reinfection were criteria, but so too was economic impact, and social stress.
There won't be any shortage of datapoints to make the collective judgement.
So what is your recommendation? Level 4 for another 2 weeks, another 4?
Because that is what the Cabinet will ask. They will want actual recommendations, not just a series of questions.
And then they have to make a judgement, because reputable people are suggesting Level 3 and others are saying stay at Level 4, at least till ANZAC day.
And despite what Iprent thinks, it is perfectly reasonable to look at the Australian experience.
Rather then look at the problem as an epidemiological problem,it is necessary to examine it as a physics problem.
The significant parameter is transport,hence constrain CV for transport by lockdown,and social distancing.As far as known CV does not have wings so transport is by aerosol,and adhesion to rough surfaces such as clothes,face ,hair etc.
Increased interaction at present is a fail.
Wayne big business and National are bullying the govt creating a panic .Rushing to open the economy to early will cost way more in the long run.Having enough testing and tracing resources is most important.after years of cost cutting /underfunding under the Key govt we will be overwhelmed if Covid gets out of Control.It could be as simple as a warmer climate in Australia has reduced the spread. Because this is a new virus we don"t have all the answers yet.Rushing to open the economy would be more economically disastrous.
Hi Wayne, thanks, great comment, you highlighted:
"Because that is what the Cabinet will ask. They will want actual recommendations, not just a series of questions. "
Take your point, but is that not what Cabinet are supposed to do? or at least the ruling party?
If, looking at the current state of NZs capability take into consideration this:
A capability (s) is made up of people, training and equipment, it takes time and effort to develop the protocols/standards associated with the training and equipment. It takes time get the right people and buy the equipment (say test kits). This does not even take into consideration the testing of the capability to iron out the rough spots. The rinse and repeat process of capability development (people, equipment, training) can be used to make our elderly care facilities safe.
Should we go move to level 3 now, personally, from observation no.
If you asked me to put a time frame, your going to hate me……
It depends (an MIT professor said to always answer lawyers this way)
For example on RNZ news at 12 they said the gold standard of testing was only a week a way.
Well given that, we need to wait at least one week, but how many weeks do we need to wait until it is a fully functioning capability that cover the required numbers to support meaningful sentinel testing? If we move from 4 to 3 we may blow our gains.
Right now, totally making it up, if in the drivers seat and listening to other posts/news, I would go for 2 more weeks at level 4.
Take care
Based on best available estimates 2weeks of level 4 is about as effective in eliminating the virus as 4 weeks of level 3 with less risks of a super-spreader mucking things up.
Based on a survey of the countries that are doing best there is one thing that works (and it is cheap): MAKE EVERYONE WEAR MASKS.
So where does everyone get an effective mask from?
In Taiwan they seem to be able to manage. It doesn't need to be an N95. We are not trying to protect the wearer.
Ardern was keen on telling people to behave as if they have the virus. Any reasonably sturdy cloth or surgical mask will prevent passing on the virus through coughing, sneezing, talking or heavy breathing. Combined with hand washing, mask wearing very much reduces the likelihood of passing on the virus to anybody but very close contacts.
I was initially skeptical, but there is enough evidence now to say that the single most important factor in Taiwan's success has been the fact that everyone wears a mask in public.
https://www.stuff.co.nz/life-style/beauty/how-to-guides/120801748/coronavirus-how-to-make-a-protective-facemask-during-lockdown
or try:
http://www.pharmacydirect.co.nz/Face-Masks/
https://new.grabone.co.nz/health-nutrition-dental/other-natural-medicine/p/disposable-face-masks-1
http://www.healthcareessentials.nz/category/2326-masks
https://www.annahstretton.co.nz/products/face-mask-pack-of-3
Same place they buy their hand sanitizer from…
joe90 "where does one get an effective mask from?"
Simple answer: China. They effectively stole our supplies of PPE.
Chinese government controlled companies were systematically stripping PPE from pharmacy and supermarket shelves here and in Australia as far back as January (I wondered at the time why these disappeared so early in the crisis). China is no friend of anyone. Sooner we form an alliance with Taiwan and recognize it as the country it is, the better.
Just one reference form a web load of the evil practises of the Chinese Empire:
https://www.stuff.co.nz/business/120927408/new-zealanders-caught-short-after-masks-sent-to-china
Do we have to let history repeat itself?
One big lesson: You can’t give up early on social distancing.
[…]
In a lot of cities, similar premature pullbacks produced a lot of “double-humped epi curves,” as Markel described them: Officials instituted social distancing measures, saw flu cases fall, then pulled back the measures, saw flu cases rise again, and reactivated the measures.
Notably, the second spike in deaths only appeared when cities removed social distancing measures, Markel’s study found: “Among the 43 cities, we found no example of a city that had a second peak of influenza while the first set of nonpharmaceutical interventions were still in effect.”
The PNAS study, which looked at 17 US cities, reported similar findings: “no city in our analysis experienced a second wave while its main battery of [nonpharmaceutical interventions] was in place. Second waves occurred only after the relaxation of interventions.”
https://www.vox.com/policy-and-politics/2020/3/24/21188121/coronavirus-covid-19-social-distancing-1918-spanish-flu
Given masks need to be changed regularly where are they going to come from
https://www.facebook.com/renilda.almanzor/videos/3014389155258670/
https://twitter.com/escapedmatrix/status/1246230749625319429
Joe 90, good article, I liked this exert from it.
The most successful approaches in 1918, Markel found in his 2007 study published in JAMA, followed those three components. First, they were early — particularly before the flu got to an inflection point in which the virus infected a certain amount of people and spread rapidly. Second, they were sustained — lasting until the virus really seemed to go away, and quickly redeployed if the virus came back.
https://www.vox.com/policy-and-politics/2020/3/24/21188121/coronavirus-covid-19-social-distancing-1918-spanish-flu
I liked the bit in bold, which would infer they had the resources and capabilities ready to go, does NZ Inc?
Also reading this from your quoted article makes me ask, does our modern day society have the stamina and motivation like the 1918 society described below in your referenced article:
"3) Seeing the effects of outbreaks drove people to serious action
The question, given the reality of how long social distancing may be necessary, is how people are going to get through this. Even beyond the damage to the economy and the loss of income involved, people are going to miss out on a lot of the experiences that enriched and validated their lives before. Experts worry social distancing, even if it’s necessary, just won’t be sustainable for weeks or months.
But people did do social distancing for weeks and months during the 1918 flu pandemic.
Markel gave one potential explanation for that: People were already very familiar with the risk if they didn’t social distance. Back then, disease epidemics and pandemics of all kinds were common. Just about everyone knew someone — from parents to aunts and uncles to children — who died of disease."
Cheers
The government has earlier stated lockdowns work in blocks of two weeks, being the understood length of time for the virus to "run it's course".
Yes, so logically level 3 will be for two such cycles, or a total of four weeks (barring a rapid rise in cases).
I see Ireland is looking at bars being closed for up to 18 months, and the UK until Christmas, Micheal Gove stating that bars and hospitality in general will be the last to be freed from restrictions.
https://www.dailymail.co.uk/news/article-8235181/Pubs-UK-shut-Christmas.html
My prediction is that Level 4 will be extended till next Monday midnight. In terms of work days for most businesses that could open, it is only two work days (Thursday and Friday) that are lost, but it extends the lockdown by five days. So a reasonable approach.
It is already evident that people are starting to practise Level 3 anyway and that will increase this coming weekend. I would say we are reaching the limit of what people will readily accept. In terms of social distancing public practise will be close to Level 3 by next Monday night.
Professor Hendy was essentially suggesting this on Morning Report.We will know in just over 3 hours.
Hendy is suggesting that an extension of two weeks,could allow for elimination.Do you want us to stumble with the end goal in sight?
https://www.stuff.co.nz/national/health/coronavirus/121123513/coronavirus-modelling-expert-says-lockdown-should-be-extended-two-weeks
I'm reminded of George Box's famously attributed comment on modelling.
"All models are wrong, but some are useful"
A lovely review of him in the link below
https://rss.onlinelibrary.wiley.com/doi/pdf/10.1111/j.1740-9713.2010.00442.x
Hendy on Morning Report also said Monday night would be a reasonable compromise. He would prefer 2 extra weeks but that next Monday night would be OK.
I'd predict the same: the exact date is less important than knowing the date. It won't be an open-ended Level 4 extension.
As mentioned on the other thread, the framing has been so successful that the NZ public are effectively volunteering for an extension of the lockdown, rather than rebelling against it as we're seeing in other countries.
The hard part of today's announcement will be the end date for the next period: the PM can (and doubtless will) emphasise that it is only provisional, but whatever date is given (e.g. 2 or 4 weeks after Level 4 ends), that will become the new expectation of "release".
Yet most New Zealanders support continuing Level 4 for longer according to the media stories I've seen this last few days, some based on polling.
Which 'people' are you thinking of?
Unless testing and tracing systems are up to scratch, then coming out Level 4 would be a bit silly – not just in terms of leaping backwards in relation to possible eradication, but also in relation to health service capacity.
Anyway. A few bases I want to cover.
Have a look at the first graph in the post and tell me that the peaks aren't 'table top mountain' peaks. In other words, in terms of infection rates/deaths, we fly up the cliff face and then spend a long time plodding down off the escarpment. And that's not quite the impression being given by media speaking of 'peaks'.
Sweden with its voluntary distancing might be getting higher death rates now, but the important number will be in the final death rates. And we won't know how Sweden has compared to (say) other Nordic countries until some time in the future. (jist sayin')
Lastly.
It might be the case that NZ is in the very unusual position of being able to possibly eradicate the virus. I can't see that being the case for places with already high numbers of infection. But assuming there is no vaccination on the horizon (a reasonable assumption), and assuming 'the rest' of the world remains chronically infected – what then for a Covid free NZ? How's that work?
" But assuming there is no vaccination on the horizon (a reasonable assumption), and assuming 'the rest' of the world remains chronically infected – what then for a Covid free NZ? How's that work?"
It works a hell of a lot better than if we dont eradicate the virus here….the specifics can wait
I agree. But still…I wonder if people are giving it any thought, and how they might feel about living in Noah Land, aye? 😉
Pretty sure many are…theres plenty of evidence of agendas at play
A trade and tourism union and free travel area with other similar countries, such as Australia and Taiwan would be a start.
Agree re Sweden: interestingly, the infection rates for all the Nordic countries, despite their vastly different approaches, are almost identical. Yes, testing rates and methods may play into that, but so does the demographic profile and so many other variables.
Hugely disagree re 'no vaccination on the horizon (a reasonable assumption)'. Its now a global effort, many many trials now progressing through the animal testing stage and about to enter the human testing stage. This virus no doubt will lead to a quantum leap in scientific knowledge.
"Agree re Sweden: interestingly, the infection rates for all the Nordic countries, despite their vastly different approaches, are almost identical."
Best you go look again…Sweden considerably worse on all measures.
https://www.worldometers.info/coronavirus/
Using the figures above in the article, Infection rates, that being as a percentage of the total population, are all about .0013 for all the Nordic countries.
Death rates are irrelevant, as reflect demographics, level of health care, heath care policies and so on.
2 key stats ..infections per million and testing per million
Sweden has the lowest (by far) testing rate yet has the highest detected case rate (double that of Finland)
It's a logarithmic graph, not a linear one.
Can you explain how that works in terms of what I'm seeing?
Am I simply not understanding how the graph should be interpreted, and the virus is perhaps fading as fast as it arrived? (All I’m seeing is a very slow decline in numbers for Italy, the US, UK, France…)
Just tends to flatten out the tops, is all.
You're comment is hardly explanatory Sacha.
Is my basic interpretation right, or is it way off the mark because of an incorrect reading of the graph? Or put another way, does the fact of the graph being logarithmic or linear make any meaningful difference to what I wrote?
The peaks are probably sharper than they look here. Sorry, day job intervenes.
Totally agree.
From the first three to four minutes of this link.
The Netherlands has tested its blood banks for the virus, and the results indicate that infection rates in the Netherlands are far higher than is being picked up by testing out in the general population.. Assuming the blood banks are a representative cross section of society (ie- absenting a reason to suspect that people donating blood should have a higher infection rate) – then the death rate as a percentage drops considerably.
Anyone know if New Zealand has tested it's banks of donated blood and compared the rate of infection detected there to the infection rate from general testing? And if that has been done, how do the numbers compare?
They have certain protections in place in NZ for blood donations eg no contact with C-19 positives, no sickness symptoms, at least 4 weeks since returned from overseas, etc.
Hmm. So perhaps in the interests of getting an accurate picture, any testing would have had to have been done on the 35 day stock that existed prior to March 23rd?
I dare say blood was never taken from people who were 'feeling off' – and that would apply in the Netherlands and elsewhere too.
Anyway, the findings in the Netherlands are interesting….and (just thinking this through as I type) – shouldn't NZ's donated blood be tested given that Covid doesn't necessarily mean that infected people exhibit symptoms?
It's a wee bit of a worry that decisions are being made on the basis of inadequate data.
I am very suspicious of the results of the pop up paknspend testing.
Personally, I'm dead keen for Level 3 as life in Lockdown for Peter and myself sees us in a less than safe living environment. For various reasons. Level three would herald the start of the'moving back to our own safer living space' process which in itself might take two weeks or more before we can go 'home's and ultimately be safer.
Putting self interest aside however, the facts are that this government has not enough data to truly know there is little if any community transmission AND with what information we do have it would seem that having frail old folks and high needs disabled sacrificed to the Virus Gods might actually be part of a worldwide plan.
I am hating Level 4. BUT, I simply don't trust that the government does in truth have the interests of this vulnerable group at heart and they might actually be safer at Level 4.
do you know if mechanics will be back at work under L3 and under what conditions? eg essential repairs only?
I don't see why mechanics can't work now, tbh, allowing self interest a free rein. In my experience the average truck and car repair shop is hardly cuddle central. Social distancing is most definitely order of the ordinary pre Virus work day. Smoko might have to be altered…but the actual work would create less of a transmission issue than what I observed last time I ventured into a supermarket.
But that's just my biased opinion.😉
Here's hoping.
the govt wanted to limit driving, so I can see why normal mechanical business would be classed as non-essential under L4. Call outs eg AA were still going afaik, but I don't know if they were doing repairs. You'd hope so.
Still sucks you weren't given access to your bus.
Starter motor (or possibly the battery) clapped out on the car last night when my partner was going to the supermarket.
But it is local, so she walked there, and I followed her on the e-bike with dual panniers and a backpack.
But I’d point this out about mechanics…
https://www.stuff.co.nz/motoring/120787609/how-to-take-care-of-your-car-during-lockdown
see https://www.stuff.co.nz/motoring/120787609/how-to-take-care-of-your-car-during-lockdown
Mechanics were essential already. But a lot of them, especially the smaller ones, closed down.
And don’t forget the dairy operators.
in my area none of dairy owners wore masks or had any precautionary measures (Perspex dividers etc.) taken other than a one customer in the shop at the time.
how we could allow dairy’s operating like this beyond any logic.